This article was updated on January 23, 2017.
The new Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) ties physicians’ payments to greater accountability of cost and quality with the introduction of two distinct pathways that adjust payment using different criteria: the Merit-Based Incentive Payment System (MIPS) and the Advanced Alternative Payment Model (APM) track. MIPS seeks to tie Medicare payments to provider performance within the fee-for-service (FFS) system, whereas the Advanced APM track encourages groups of providers to shift away from FFS to delivery models where physicians assume more accountability and risk for cost and quality of care through APMs, providing lump-sum incentive payments for the initial years of the program for early adopters of such models.
Transition from current payment programs
MIPS replaces the three payment programs that eligible professionals (EPs)1 are subject to in the performance year 2016 under Medicare FFS, including:
1. Physician Quality Reporting System (PQRS): A penalty-only program for reporting quality measures each year. EPs will be penalized -2% of their Medicare Part B payments in 2018 if they fail to report in 2016 with no potential for bonuses.
2. Value Modifier (VM): A two-sided program based on quality and cost performance of an attributed population. EPs in practices with at least 10 EPs can have a penalty of up to -4% and a bonus of up to +4X% of their Medicare Part B payments in 2018 based on their performances in 2016, and EPs with fewer than 10 EPs in their practices can have a penalty of up to -2% and a bonus of up to +2X% of their Medicare Part B payments in 2018 based on their performances in 2016.2
3. Meaningful Use (MU): A penalty-only program for those providers who fail to meet standards surrounding the meaningful use of electronic health records. EPs can have a penalty of up to -4% in 2018 based on failing to attest to MU in 2016 with no potential for bonuses.
These programs are additive, meaning that in the 2018 payment year, some EPs will have a potential penalty of up to -10% and a potential bonus of up to +4X%. All of these programs will be replaced with the MACRA-defined programs with adjustments for the 2019 payment year based on the 2017 performance year. Under MIPS, practices will receive one Composite Performance Score (which we refer to as final score, described below), which takes into account multiple cost and quality dimensions.
Physicians have been paid under the performance-based programs cited in the “Transition from current payment programs” sidebar since 2015, but MACRA creates an opportunity for physicians and other professionals to choose how they participate in the Medicare-FFS payment programs. While many providers may choose to pursue qualification in the Advanced APM track versus participating in MIPS, there are also several choices that providers can make to optimize MIPS performance. In this paper, we will cover the transition from the current payment programs to MIPS, review the MIPS inclusion criteria, discuss the final score, demonstrate how the final score leads to the determination of the MIPS adjustment factor, and explore the effect of changing practices on both the final score and MIPS adjustment factor.
This paper reflects information provided from the following sources:
- The MACRA proposed rule released in April 2016
- The 2017 Physician Fee Schedule proposed rule released in July 2016
- The MACRA final rule released in October 2016
Note that in all cases, any materials cited from the MACRA proposed rule have been updated to reflect the final rule, such that all information in this paper is current as of November 2016.
Overview of MIPS
MIPS represents a replacement for several existing payment programs that certain physicians and nonphysician practitioners are subject to under Medicare FFS (see the "Transition from current payment programs" sidebar). With MIPS, the Centers for Medicare and Medicaid Services (CMS) is taking a step toward tying payment to quality and cost as opposed to simply the volume of services rendered. MIPS will first be implemented in 2019 (based on performance as measured in 2017). According to the final rule, a transitional year will allow providers to choose between several levels of participation for the 2019 payment year, with more complete implementation in the following 2020 payment year. CMS has indicated that additional rulemaking in 2017 may adjust the implementation parameters for the 2020 payment year as an additional transition period. Certain clinicians will be exempt from MIPS for reasons described below.
Under MIPS, most physicians and nonphysician practitioners will be measured on a collection of quality and cost metrics. Their performance on these metrics will be translated into a final score. Based on the final score, each payment made to the physician or nonphysician practitioner will be subject to an upward or downward adjustment. In an effort to achieve budget neutrality, upward MIPS adjustments can be scaled to balance the downward adjustments. There is also a pool of additional money available to be paid as exceptional performance adjustment payments to top MIPS performers.
MIPS-eligible clinicians
Most eligible clinicians (see the "eligible clinicians" sidebar) will be participating in MIPS,3 though there are exceptions. They include the following:
- Newly enrolled Medicare clinicians: Clinicians who are in their first Medicare Part B participation calendar years are excluded from MIPS participation.
- Clinicians below Medicare patient volume threshold: Clinicians with less than or equal to $30,000 of Medicare billing charges or who are providing care for 100 or fewer Part B-enrolled Medicare beneficiaries are defined as low volume in the MACRA final rule and are as such exempt from MIPS reporting.4
- Qualifying APM Participants (QPs): QPs are excluded from MIPS (please see Advanced APMs and Qualifying APM Participant status).5 Partial Qualifying APM participants (Partial QPs) can choose whether or not to receive a MIPS adjustment factor.6
Eligible clinicians
The final rule uses the term “eligible clinician,” which has the same meaning as the term “eligible professional” in other aspects of Medicare. It can include both physicians and other practitioners. In the 2019 and 2020 payment years, "eligible clinician" refers to physicians, nurse practitioners (NPs), physician assistants (PAs), clinical nurse specialists (CNSs), and certified registered nurse anesthetists (CRNAs).7 Beginning in 2021, the U.S. Department of Health and Human Services (HHS) may specify other types of practitioners, whose payments are regulated under the Physician Fee Schedule, as eligible clinicians. Specific examples of additional practitioner types provided in the statute are certified nurse-midwives, clinical social workers, clinical psychologists, registered dietitians or nutritional professionals, physical or occupational therapists, qualified speech-language pathologists, and qualified audiologists.8
MIPS Final score
Every MIPS-eligible clinician will receive a MIPS final score. The final score is defined as a value between 0 and 100 that will be calculated for every MIPS-eligible clinician and will be used to determine payment adjustments in the MIPS program.9 The final score is composited from four performance categories, three of which are directly related to the current programs that MIPS replaces. The four categories are:
1. Quality: Similar to the quality composite of the VM program and utilizing PQRS submission mechanisms.
2. Resource use (referred to as “cost”): Similar to the cost composite of the VM program. The final rule indicates the calculation of this category will change in the future.
3. Meaningful use of CEHRT (referred to as “advancing care information”): Related to meaningful use, but with significant changes.
4. Clinical practice improvement activities (referred to as “improvement activities” ): New category.
The weights of each performance category change over time and are shown in the table in Figure 1.10
Figure 1: Final score performance category weights by year
| MIPS performance category | MIPS-eligible clinicians not in a MIPS APM | ||
| 2019 | 2020 | 2021 and subsequent years | |
| Quality | 60% | 50% | 30% |
| Cost* | 0% | 10% | 30% |
| Advancing Care Information (ACI) | 25% | 25% | 25% |
| Improvement Activities (IA) | 15% | 15% | 15% |
| *Note that while the cost category will not be required nor will it affect the final score for 2019 payment, CMS will still provide feedback on 2017 performance. | |||
MIPS-eligible clinicians can submit MIPS data as individuals or as a group, which is defined by TIN (see the "Data submission by groups" sidebar). The data submission deadline for all categories is March 31 following the close of the performance year.
Eligible clinicians who are participating in certain APMs, called “MIPS APMs” (see the MIPS APMs sidebar), have different category weights, shown in the table in Figure 2.
Figure 2: Final score performance category weights for MIPS APM participants
| MIPS performance category | MIPS-eligible clinicians participating in MSSP or NGACO | MIPS-eligible clinicians participating in any other MIPS APM (exclusive of MSSP and NGACO) | ||
| 2019 | 2020 and subsequent years | 2019 | 2020 and subsequent years | |
| Quality | 50% | Not yet defined | 0% | Not yet defined |
| Cost | 0% | 0% | ||
| Advancing Care Information11 | 30% | 75% | ||
| Improvement Activities | 20% | 25% | ||
| MSSP: Medicare Shared Savings Program. NGACO: Next Generation Accountable Care Organization. | ||||
Data submission by groups
Submitting as a group may require less data collection and submission, but aggregates the performance of all eligible clinicians across the TIN for all MIPS performance categories. For example, if a practice elected to submit quality measures as a group, then each eligible clinician in the TIN would have the same final score and, therefore, the same MIPS adjustment.
MIPS APMsCMS has defined the following MIPS APMs:12
- Medicare Shared Savings Program (MSSP) all tracks
- Next Generation Accountable Care Organization Model (NGACO)
- Comprehensive ESRD Care (CEC) all options
- Comprehensive Primary Care Plus (CPC+)
- Oncology Care Model (OCM) all tracks
- Vermont Medicare ACO Initiative
While participants in these MIPS APMs may not meet all the requirements to move into the Advanced APM track, there are several key differences in the final score calculation and reporting for these clinicians.
According to the final rule, reporting requirements differ for MIPS APM participants.
Eligible clinicians who participate in a MIPS APM will receive 50% credit for their IA score. This means that they will only need 30 additional points to receive the highest possible IA score (100%).
Performance category: Quality
Quality measures will largely be based on current measures used in PQRS and VM. In the final rule, CMS plans to use a mix of reported and claims-based measures for this category. Final quality metrics will be published no later than November 1 of the year prior to the performance year.
Most eligible clinicians will submit at least six measures that must include one cross-cutting measure (if the eligible clinician is patient-facing13) and an outcome measure if available. If an outcome measure is not available to the clinician or group, then the clinician or group would report on a high-priority measure in place of the outcome measure (high-priority measures are identified in the final rule as outcome, appropriate use, patient safety, efficiency, patient experience, and care coordination measures). If a clinician or group chooses to report a specialty-specific measure set that has less than six measures, they would report on all of the available measures including an outcome measure, or, if an outcome measure is unavailable, report another high priority measure, within the set and a cross-cutting measure if they are a patient-facing MIPS-eligible clinician.
In addition to the points the clinician receives on the measures, the clinician can be eligible to receive bonus points for reporting on high-priority measures in addition to the one required outcome measure. These bonus points cannot exceed a cap, which is finalized as 10% of the denominator of the quality performance category score.
Groups with at least two MIPS-eligible clinicians can voluntarily elect to participate in the Consumer Assessment of Healthcare Providers and Systems (CAHPS) survey to comply with the quality reporting requirements of MIPS. If elected, they must use a CMS-approved survey vendor.14 The CAHPS survey for MIPS counts as one cross-cutting and/or patient experience measure and the group would be required to submit at least five other measures through another data submission mechanism.
In addition to the six reported measures, clinicians and groups will also be scored on three population-based measures that do not require data submission. These measures are:
1. Acute Conditions Composite, including Bacterial Pneumonia (PQI 11) (NQF 0279), Urinary Tract Infection (PQI 12) (NQF 0281), and Dehydration (PQI 10) (NQF 0280)15
2. Chronic Conditions Composite, including Diabetes (PQI 03, 01, 14,16) (NQF 0274, 0272, 0285, and 0638), Chronic Obstructive Pulmonary Disease (COPD) or Asthma (PQI 5) (NQF 0275), and Heart Failure (PQI 8) (NQF 0277) 16
3. 30-day All-Cause Hospital Readmission Measure17
Practices with 15 or fewer MIPS-eligible clinicians will be excluded from the 30-day All-Cause Hospital Readmission measure. Therefore, practices with 16 or more MIPS-eligible clinicians will typically have nine measures and those MIPS-eligible clinicians who are in practices with 15 or fewer MIPS-eligible clinicians will typically have eight measures.
Performance category: Cost
This measure has no weight in the final score for the 2017 performance year/2019 payment year. However, it will still be calculated and will initially be based on two of the six VM measures currently utilized in the VM program along with up to 41 proposed episode-based measures, but are expected to evolve over time. The total per capita costs include both Medicare Part A and Part B payments of the attributed population, but CMS is evaluating the future inclusion of Medicare Part D as directed in the MACRA law. The two current cost measures to be used starting in 2018 are as follows:18
1. Total per capita costs for all attributed beneficiaries
2. Medicare spending per beneficiary (MSPB), which is defined as expenditures in the period three days prior to a hospital admission through 30 days post-discharge19
The law also calls for modifications to the current attribution process used in VM to address concerns that the current rules do not accurately link the services to the correct provider. The development of care episode, patient condition, and patient relationship codes will seek to inform cost measures under this performance category. The MACRA statute states that 1) national provider identifier (NPI) numbers, 2) care episode and patient condition codes, and 3) patient relationship codes are required for all claims submitted after January 1, 2018.20
CMS also plans to use the same methodologies for payment standardization and risk adjustment for these measures for the cost performance category as are defined for the VM.
Performance category: Advancing care information (ACI)
The ACI performance category was created to encourage meaningful use of health information technology, and it replaces the Meaningful Use program, which was a penalty-only program that imposed penalties on providers who did not meet certain criteria.
In the final rule, CMS has relabeled “meaningful use” (from the existing program and labeled under the statute) as “Advancing Care Information” to reflect the changes made to the program.21 Namely, rather than the all-or-nothing score given under the current system, CMS has finalized that clinicians could achieve partial credit based upon their degrees of participation.22 Its weight as a proportion of the final score for most MIPS-eligible clinicians is 25%.23
In the final rule, performance would be assessed using a base score (worth up to 50%), performance score (worth up to 90%), and bonus points (worth up to 15%). This means the score can be up to 155%, but any score above 100% will receive the maximum ACI points toward the final score.24 If a clinician earns fewer than 100%, the ACI points for the final score will decline proportionately. Further discussion of each of the ACI scores follows.
-
Base score. To receive the maximum 50% base score, eligible clinicians would need to provide either the numerator and denominator or a yes or no answer to the following objectives and measures:
1. Protect patient health information (yes required): Clinicians must meet this measure in order to receive any ACI points.
2. Electronic prescribing (numerator/denominator).
3. Patient electronic access (numerator/denominator).
4. Send a summary of care (numerator/denominator).
5. Request/accept a summary of care (numerator/denominator).
The 2017 transition measures include 1-3 above as well as health information exchange. - Performance score. This is worth up to 90%. To receive credit for this category, eligible clinicians will be measured based on their performance rate for reported numerators and denominators included in the performance score. Each measure is worth from 10 to 20 percentage points.
- Bonus points. Clinicians can receive 15 bonus percentage points for reporting to public health and clinical data registries beyond the immunization registry (5%) and reporting “yes” to completion of at least one specified improvement activity using CEHRT (10%).
Unlike the current Meaningful Use program, ACI permits clinicians to choose between individual and group reporting and scoring.
Performance category: Improvement activities (IA)
The focus of this new category is on assessing the effort professionals put into engaging in clinical practice improvement activities. These activities include expanded practice access (e.g., same-day appointments for urgent needs), population management, care coordination, beneficiary engagement, patient safety and practice assessment, participating in APMs, promoting health equity and continuity, achieving health equity, integrated behavioral and mental health, and emergency response and preparedness.
Clinicians in a certified patient-centered medical home (PCMH) or comparable specialty practice will be given the highest potential score for this category in the performance period.25 The PCMH must be nationally recognized through accreditation—including 1) the Accreditation Association for Ambulatory Health Care, 2) the National Committee for Quality Assurance (NCQA) PCMH recognition, 3) the Joint Commission Designation, or 4) the Utilization Review Accreditation Commission (URAC)—or be a Medicaid Medical Home Model, or have received NCQA recognition as a Patient-Centered Specialty Practice. The final rule acknowledges that practices may receive PCMH designation at a practice level and that individual TINs may be composed of both undesignated practices and practices that have received designation. The final rule indicates that for MIPS-eligible clinicians who choose to report at the group level, reporting is required at the TIN level.
Clinicians who do not participate in a PCMH (or equivalent) will choose from the over 90 activities listed as IAs.26 High-weighted activities are worth 20 points each and medium-weighted activities are worth 10 points each. In order to achieve the highest possible IA score in the final score (100% of the IA category), clinicians must earn 60 points from some combination of these activities. To receive credit for engaging in approved IAs, clinicians or groups must perform the activities for at least 90 days during the performance period.
Groups with 15 or fewer eligible clinicians, groups in rural areas or geographic Health Professional Shortage Areas (HPSAs), and non-patient-facing MIPS-eligible clinicians or groups are required to perform two IAs (either medium or high weight) to receive the highest possible score (100%). Completion of one IA will result in a 50% IA score for the final score.
Final score to MIPS adjustment
Performance thresholds
Prior to the performance period, the HHS Secretary will establish the performance threshold used for determining MIPS adjustment factors. It is important to note that the standard will be set based upon previous performance (as compared with a set expected performance standard) and participating physicians will know the threshold in advance of the performance period itself. For the first two years of MIPS, this process will differ from when the program has been implemented over a longer period.
In the final rule, CMS has implemented a program referred to as “pick your pace” within the MIPS track for payment year 2019 (with performance to be assessed in 2017). Specifically, in 2017, providers can choose one of the following options:
- Don’t participate: Providers who send in no data in 2017 will receive the maximum -4% payment adjustment in 2019.
- Submit something: If providers submit a minimum amount of 2017 data (only one measure, for example), they will be insulated from downward payment adjustments.
- Submit a partial year: If providers submit 90 days of 2017 data, they may earn a neutral or small positive payment adjustment for 2019.
- Submit a full year: If providers submit a full year of 2017 data, they can earn a moderate positive payment adjustment.
The pick your pace program will only be available for the first year of MACRA implementation (performance year 2017/payment year 2019).
Given the pick your pace program, CMS has set the performance threshold for payment year 2019 at 3 points (with clinicians who achieve a final score of 70 or higher being eligible for the exceptional performance adjustment).27 For 2020, the performance threshold calculation has not yet been outlined and will likely be higher, given that 2019 is artificially low because of the transition period.
In 2021 and subsequent payment years, the performance threshold for a year must be either the mean or median (as selected by the HHS Secretary and which may be reassessed every three years) of the final score for all MIPS-eligible clinicians for a prior period specified by the Secretary.
Eligible clinicians with a final score equal to the performance threshold will not receive an adjustment. Eligible clinicians with a final score above the performance threshold will receive an upward adjustment, while those with a final score below the performance threshold will receive a downward adjustment.
Calculation of the payment adjustment from the final score
The adjustment factor for each MIPS-eligible clinician will be determined with a linear sliding scale from zero to 100, with zero being the maximum downward adjustment and 100 being the highest possible upward adjustment. Prior to applying the linear sliding scale, two modifications must be applied. The first is the application of the maximum downward adjustment. Those with a final score between zero and one-quarter of the performance threshold will receive the maximum negative MIPS adjustment factor for the MIPS payment year. Next, all positive MIPS adjustment factors are multiplied by the scaling factor, which will be between zero and 3. Only those eligible clinicians with a final score of exactly the performance threshold would receive no adjustment.
In payment years 2019 to 2024, those eligible clinicians achieving an upward adjustment with the highest final score are eligible for an exceptional performance payment. CMS will establish an “additional performance threshold” that defines which eligible clinician will receive the exceptional performance payment. The additional performance threshold is set at the 25th percentile of the scores above the performance threshold. For a visual representation, see Figure 3 below.
Figure 3: MIPS adjustment
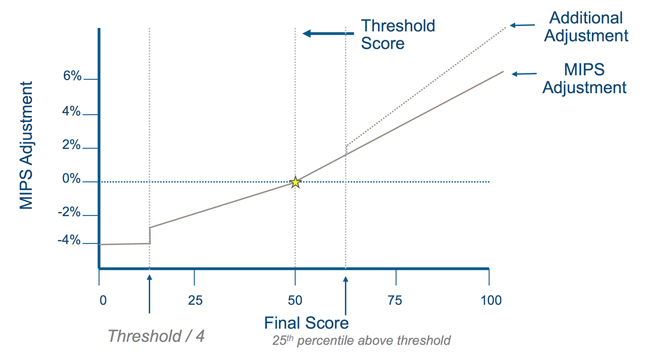
Those eligible clinicians with a final score of at least the additional performance threshold (the 25th percentile above the final score threshold score, as shown by the rightmost vertical line in Figure 3) will receive a 0.5% adjustment and the eligible clinicians with the maximum final score will receive an exceptional performance adjustment not to exceed 10%. There will be a scaling factor applied to the exceptional performance adjustment to ensure that the aggregate incentive payments for exceptional performance do not exceed $500 million in each year. This scaling factor is to be between zero and 1 to achieve this goal, so it can only have the effect of decreasing exceptional performance adjustments and is denoted as Y in Figure 4.
Translating a final score to a MIPS adjustment
Once a final score is determined for each TIN/NPI, the final score will be translated to a MIPS adjustment. The MIPS adjustment factor will be applied to all payments in a given payment year, starting in 2019. The performance year is always two years prior to the payment year. The potential upward/downward MIPS adjustment grows from -/+4% to -/+9% (see the table in Figure 4). Upward adjustments will be multiplied by a scaling factor (denoted as X in Figure 4) between zero and 3 (calculated each year to ensure budget neutrality). This means that, in payment year 2019, the potential upward adjustment ranges from zero (if there are no downward adjustments) to 12% (if there are sufficient downward adjustments to merit a scaling factor of 3).
In addition to the adjustment factor, the statute provides for an exceptional performance adjustment as described above. This performance adjustment will be applied in a linear fashion so that those with a top final score will receive a 10Y% increase and those at the additional performance threshold will receive a 0.5Y% increase.
Figure 4: MIPS payment adjustments by year
| Payment year | Performance year | Maximum downward adjustment | Maximum upward adjustment* | Maximum exceptional performance adjustment** | Total potential adjustment range |
| 2019 | 2017 | -4% | +4X% | +10Y% | -4% to +22% |
| 2020 | 2018 | -5% | +5X% | +10Y% | -5% to +25% |
| 2021 | 2019 | -7% | +7X% | +10Y% | -7% to +31% |
| 2022 to 2024 | 2020 | -9% | +9X% | +10Y% | -9% to +37% |
| 2025 and beyond | 2023 and beyond | -9% | +9X% | - | -9% to +27% |
| *Each year, the upwards adjustment scaling factor "X" will be calculated to determine the actual percent of the adjustment. The scaling factor can be between zero and 3 and is designed to be budget-neutral in regard to the downward adjustments. | |||||
| **Each year, the exceptional performance adjustment scaling factor "Y" will be calculated so that the total exceptional performance adjustment payments do not exceed $500 million. The scaling factor can be between zero and 1. | |||||
Maximizing MIPS opportunity
The MIPS program represents an evolution of current payment programs for professionals paid under Medicare Part B. Eligible clinicians can report as individuals, groups, or as part of certain APMs. There are pros and cons to each approach and clinicians should evaluate their options based on the cost of compliance and the likelihood of earning an incentive. Milliman has tools, data, and expertise to help clinicians understand their options and select the participation level that optimizes the financial return and minimizes the financial risk for a given scenario.
1Each program defines eligible professionals as some collection of physicians and other clinicians whose payments are governed by the Physician Fee Schedule.
2From proposed 2017 PFS, page 802. Practice is defined by tax identifier number (TIN). Upward adjustments are subject to budget neutrality, which is maintained by the scaling factor “X” calculated prior to the start of the payment year.
3Please see Advanced APMs and Qualifying APM Participant status paper for description of how MIPS versus APM status is determined.
481 Fed. Reg. 77064 (November 4, 2016).
581 Fed. Reg. 77036 (November 4, 2016).
681 Fed. Reg. 77062 (November 4, 2016).
7MACRA: Pub. L. 114-10 Sec. 101(c)(1) (April 16, 2015), Soc. Sec. Act § 1848(q)(1)(C).
11The Advancing Care Information weights may decrease to as low as 15% if determined that 75% of eligible clinicians are meaningful users.
12Of note, all currently available Advanced APMs are also MIPS APMs. Please see Advanced APMs and Qualifying APM Participant status for further discussion of Advanced APMs.
13CMS proposes defining non-patient-facing MIPS-eligible clinicians as those clinicians or groups that bill 100 or fewer patient-facing encounters during a performance period. Patient-facing encounters will be defined as general office visits, outpatient visits, and surgical procedure codes, and a proposed list of patient-facing encounter codes will be published on the CMS website.
1481 Fed. Reg. 28183 (May 9, 2016).
15For those with at least 20 cases.
16For those with at least 20 cases.
17For those with at least 200 cases.
1881 Fed. Reg. 28198 (May 9, 2016).
19The use of the MSPB measure for MIPS will have two minor technical adjustments as compared to its current use in the VM.
2181 Fed. Reg. 28163 (May 9, 2016).
2281 Fed. Reg. 28164 (May 9, 2016).
23MACRA enables the HHS Secretary to reduce this weight to no less than 15% if 75% of eligible clinicians have successfully met ACI requirements.
24Advancing Care Information Fact Sheet. Available here.
25MACRA: Pub. L. 114-10 Sec. 101(c) (April 16, 2015).
About the Author(s)
MIPS adjustment overview
This paper covers the transition from current payment programs to the Merit-Based Incentive Payment System (MIPS), reviews the MIPS inclusion criteria, discusses the Composite Performance Score (CPS), demonstrates how the CPS leads to the determination of the MIPS adjustment factor, and explores the effect of changing practices on both the CPS and MIPS adjustment factor.