What's driving the high risk score trend in the 2018 Advance Notice?
Introduction
The 2.1% Medicare fee-for-service (FFS) 2016 medical risk score trend surprised many, and was the primary driver behind the increase in the Part C FFS normalization factor proposed in the 2018 Advance Notice.1 If implemented, this will result in a 1.9% reduction to Medicare Advantage funding.
The trend differs from the relatively flat trends observed for the previous four years, as shown in the graph in Figure 1.
Figure 1: Medicare FFS CMS-HCC Risk Scores*
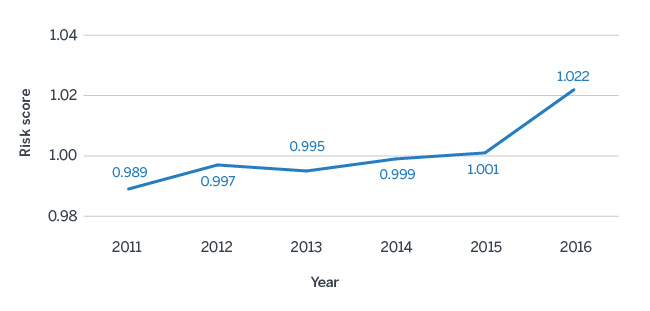
*Per page 30 of the 2018 Advance Notice.
To validate and understand the 2016 trend, we calculated Medicare FFS risk score trends and Hierarchical Condition Category (HCC) changes using the Medicare 5% Sample.
Watch for follow-up articles as we continue the analyses discussed in the body of this article.
Six key HCCs drive risk score trend
Our risk score trend analysis is consistent with the trend in the Advance Notice. In addition, we identified the HCCs shown in Figure 2 as the key drivers of the 2016 risk score trend.
Figure 2: Major HCC Contributors to 2016 Risk Score Trend
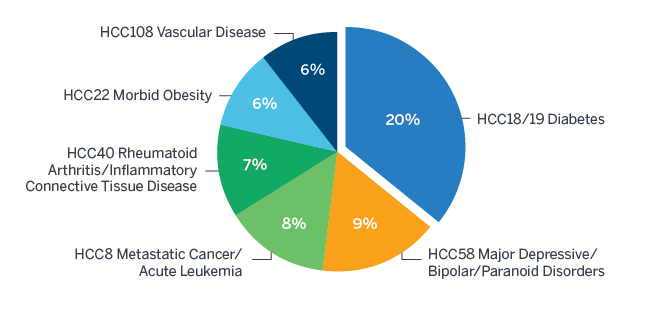
Diabetes with Chronic Complications (HCC18) had the most significant HCC increase, while Diabetes without Complications (HCC19) decreased to partially offset it. We suspect this may be related to the conversion from ICD-9 to ICD-10 diagnosis codes effective October 2015.
We will provide additional insight concerning the FFS trends, HCC changes, and the impact of the ICD-9 to ICD-10 conversion as we continue our research.
Risk score trend implications
FFS normalization
The Centers for Medicare and Medicaid Services (CMS) calibrated the CMS-HCC risk score model to produce a 1.0 risk score using 2015 FFS risk scores. Because the average risk score changes after the model calibration year, due to coding and population changes, CMS applies a normalization factor so the average risk score remains at 1.0 for each projection year.
CMS reviews risk scores over a five-year period in projecting the FFS normalization factor; therefore, the impact of the 1.022 risk score for 2016 drives an increase in the 2018 FFS normalization factor to 1.017. We estimate the FFS normalization would be 1.009 if 2016 were excluded. As FFS risk score trends increase, the FFS normalization factor will also increase, which will result in decreases to the Medicare Advantage risk scores and revenue.
Additional information on the development of the normalization factor can be found on pages 29 to 34 of the 2018 Advance Notice.
MAO risk scores
In addition to regular monitoring, we recommend that Medicare Advantage Organizations (MAOs) review their 2016 and 2017 risk score trends, and identify the underlying drivers of any changes. This will be key in setting 2017 and 2018 risk score trends for the 2018 bid development. Also, to the extent that MAO risk scores trends are lower than FFS trends, the MAO will see unfavorable revenue changes. This scenario is likely in a situation where the increase in the FFS risk score is driven by increased coding accuracy that an MAO has already realized via chart reviews or other interventions.
Methodology
We developed our risk score trends using diagnosis data from the 2011 to 2015 Medicare 5% Sample data, after filtering out claims not acceptable for risk adjustment, per CMS guidance. We excluded end-stage renal disease (ESRD), hospice, Medicaid, institutional, and Medicare Advantage members, as well as members who were not enrolled with Medicare FFS for both Part A and Part B during the entire 12-month diagnosis period. We based the risk scores on the Payment Year 2017 CMS-HCC model and calculated them using software provided by CMS. We tested alternate scenarios using different populations as well as the CMS-HCC model used for Payment Year 2016. The overall trend results for all scenarios were largely consistent with the Advance Notice.
We relied on data and other information provided by CMS, specifically the 5% Sample, the CMS Risk Participant Guides, the 2018 Advance Notice, and other CMS memos and publications. While we did not audit or verify this data and other information, we did not identify issues with the sources.
About the authors
Darcy Allen, Karin Cross, and Rob Pipich are consultants in Milliman’s Philadelphia office, with over 45 years of combined Medicare experience. Rob Pipich is a member of the American Academy of Actuaries and meets the Academy’s qualification standards. The article reflects the authors’ findings and opinions.
1“Advance Notice of Methodological Changes for Calendar Year (CY) 2018 for Medicare Advantage (MA) Capitation Rates, Part C and Part D Payment Policies and 2018 Call Letter”, published on February 1, 2017. https://www.cms.gov/Medicare/Health-Plans/MedicareAdvtgSpecRateStats/Downloads/Advance2018.pdf
About the Author(s)
What's driving the high risk score trend in the 2018 Advance Notice?
After calculating the Medicare fee-for-service risk score trends and Hierarchical Condition Category (HCC) changes using the Medicare 5% Sample, we determined that there are six key HCCs driving those trends.