Transparent cost network: A practical consumer-driven healthcare solution
In no other area of our economy do consumers receive services where they do not know the cost in advance and are not able to make comparisons to alternative suppliers. As a result, healthcare provider costs have remained immune from the economic forces that could control them. This immunity has contributed to greatly increasing provider costs, a major component in today’s rising healthcare costs.
The lack of price information stems from the confidential nature of negotiations between providers and payors. Providers compete with each other trying to get the highest payment from payors, and payors compete with each other trying to set the lowest payments to providers. In hopes of getting the best deal, both providers and payors want their negotiated rates to be kept confidential. Information is kept from the consumer that is necessary to make the best choices and drive an improved market.
A transparent cost network is designed to break down this limitation, giving consumers the price information they need to make informed decisions. Payors that can deliver this valuable product offering to consumers will likely gain market share for this lower-cost product.
What is a transparent cost network?
A transparent cost network (TCN) makes cost information available to members by provider and procedure along with the members’ resulting cost sharing. Members are able to compare providers directly to see what they will pay in advance of the service being performed.
Currently, the market is a hodgepodge of fee schedules and discounts, making it difficult to compare provider costs and estimate fees in advanced. By contrast, a TCN will use a single base fee schedule for all providers in an area. The amount paid to providers is set as a multiple of the schedule, which the payor negotiates with each provider.
Use of a base schedule also reduces administrative costs for payors and providers. This approach simplifies the negotiation process for both parties because the negotiation is limited to a single number, the multiple of the base fee schedule. It also reduces the cost of claim adjudication and provider auditing of payments received.
Glossary
ACO: Accountable care organization. A healthcare provider organization that is reimbursed based on efficiency and quality.
APR-DRG: All Patient Refined Diagnosis-Related Group.
ASC: Ambulatory surgery center—a facility for outpatient surgery.
CDHP: Consumer-driven health plan. Health insurance plans that utilize personal savings accounts and provide tax benefits to employees or employers or both.
DRG: Diagnosis-Related Group. A classification system for hospitalizations.
HCPCS: Healthcare Common Procedure Coding System. Coding system used by physicians and other healthcare providers.
MS-DRG: Medicare Diagnosis-Related Group.
RFP: Request for proposal.
TRICARE DRG: TRICARE Diagnosis-Related Group. TRICARE is a U.S. Department of Defense healthcare program that provides civilian health benefits for military personnel, military retirees, and their dependents.
Easy and effective member education is made possible by the TCN because the costs of all services by providers can now be easily shown. This information can also be used after services are performed to educate members on how they could have used the reports to save a specific dollar amount if they had made another choice.
Natural evolution of current consumer transparency efforts
A number of studies have demonstrated the range of price variation within healthcare markets (see Resources below for a few recent articles). This wide price variation led to the creation of tiered networks and consumer-driven health plans (CDHPs). However, existing contract structures made it difficult for payors to communicate relative costs to members. Tiered networks can show relative costs broadly, but do not inherently distinguish the relative costs of providers within each network tier. Payors that have tried to communicate relative cost specific to each provider have found it difficult because the relative cost of providers varies by service. To simplify the communication and prevent members from needing to know specific services prior to evaluating providers, payors have used broader approaches such as dollar symbols, which are valuable rules of thumb, but cannot communicate exact relativities for specific services nor demonstrate the potential cost savings from using lower-cost providers (see Resources for additional information).
With a TCN, the relative cost of each provider can be communicated using a single number (the multiplier of the base schedule) and this relativity will apply regardless of the service. This allows members to evaluate the cost/quality trade-off for healthcare services in the same manner as for any other purchase. Furthermore, since the exact service does not need to be known, this evaluation can be done even before the need for any service arises, which will allow members to make more informed decisions even for emergency healthcare services.
Implementing a transparent cost network
The following approach is recommended for implementation:
1) Gain the support of one or more large employer groups
If one or more large employers can be sold on the concept, that support will help to encourage providers to participate.
2) Expand communication to build interest and incent providers to participate
Multiple avenues should be pursued; options include: issue a press release, get a local reporter to follow the implementation, present to employer/industry organizations. Publicity and employer support may be strong motivators for provider participation.
3) Develop the base fee schedule
We recommend using an objective base fee schedule, such as Medicare or using the Milliman GlobalRVUs™. The inpatient schedule should be based on diagnosis-related groups (DRGs) but could use MS-DRGs, TRICARE DRGs, or APR-DRGs. The outpatient hospital and professional schedules should be HCPCS-based. The base schedule should be independent, transparent, and easy to understand so that providers trust they are not being manipulated by the payor. It is critical that the same base fee schedule be used by all providers in the TCN.
4) Establish provider reimbursement using the base fee schedule with multiplier
Reimbursement can be negotiated with providers through an RFP process. The payor should calculate their current contract equivalent multiple of the base schedule and encourage the provider to respond with a lower multiple to attract market share.
5) Select a few simple benefit designs; deductible and coinsurance benefit plans that reflect actual fee schedule differences in member cost sharing are necessary
Simplicity is the key in benefit design, both for member motivation and for reducing costs. Member cost sharing based on coinsurance rather than copays connects provider prices with the member’s out-of-pocket expenses, creating a critical motivator for the member to find the lowest cost provider. A high out-of-pocket maximum (e.g., $5,000 to $10,000) is recommended to ensure that the member’s connection to the cost is meaningful.
6) Create effective member reporting
Reporting serves to both educate members and support them on an ongoing basis as they change their behavior and learn to check prices before seeking services—as is done in most other industries. The effectiveness of the reporting will heavily impact the success.
A good reporting solution would be to create a website where a member can enter a service (e.g., surgery or imaging procedure) and the site returns a comparison of providers, showing prices and member cost sharing (see figure 1).
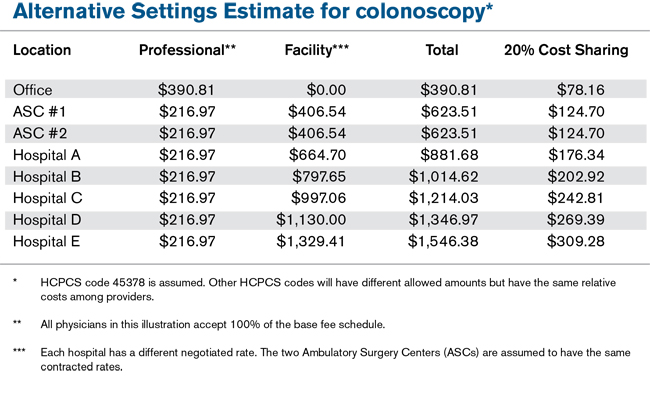
Similar reports should be provided retrospectively after a member receives services. Showing members how they could have saved money if they had selected more cost-effective providers can be very effective.
Other considerations
The transparent cost network described above focuses on costs but should incorporate efficiency, quality, and patient satisfaction into member reporting because these factors could play a role in the member’s decision on which providers to use. Many payors already have fairly mature provider quality and patient satisfaction information available to their members. The TCN will enable members to make a more complete evaluation of their provider choices.
Medical homes and accountable care organizations (ACOs) can be excellent vehicles to align the incentives for providers to work with patients to make the most cost-effective choices. The TCN would make it easier to share unit cost and efficiency comparisons for specialist and hospital referral options. If both members and their providers are incented to reduce costs and understand the cost impact of various options, healthcare costs can be reduced.
Resources
Price Variation
Ginsburg, P.B. (November 2010). Wide Variation in Hospital and Physician Payment Rates Evidence of Provider Market Power. HSC Research Brief No. 16, Center for Studying Health System Change. Retrieved October 10, 2011, from http://www.hschange.org/CONTENT/1162/.
Massachusetts Division of Health Care Finance and Policy (May 2011). Massachusetts Health Care Cost Trend: Price Variation in Health Care Services. Retrieved October 10, 2011, from http://www.mass.gov/Eeohhs2/docs/dhcfp/cost_trend_docs/cost_trends_docs_2011/
price_variation_report.pdf.
Medicare Payment Advisory Commission (MedPAC, June 2011). Report to the Congress: Medicare and the Health Care Delivery System. Chapter 7: Variation in Private Sector Payment Rates. Retrieved October 10, 2011, from http://www.medpac.gov/documents/Jun11_EntireReport.pdf.
Price Transparency
The Rhode Island insurance commissioner’s office prepared an easy-to-read summary of payor efforts and state initiatives: Rhode Island Health Insurance Commissioner (2006). Transparency in Health Care; Lessons From Other States. Retrieved October 10, 2011, from http://www.dbr.state.ri.us/documents/divisions/healthinsurance/transparency_lessons.pdf.
The National Conference of State Legislatures has a more comprehensive summary on their website of federal and state efforts: National Conference of State Legislatures (December 2010). State Legislation Relating to Transparency and Disclosure of Health and Hospital Charges. Retrieved October 10, 2011, from http://www.ncsl.org/default.aspx?tabid=14512.