Want to manage employer healthcare costs? It starts with managing utilization
The urgent desire to stem the escalating cost of healthcare is nothing new to U.S. businesses. In the last decade, plan sponsors have put in place a range of cost-cutting measures and approaches to reduce the impact of rising healthcare costs on their bottom line, only to watch costs continue to rise. 2010 promises to be no different, with healthcare costs for the typical American family of four set to increase by 7.8% to $18,074.1 The increase of more than $1,300 from 2009 is the highest we have seen since we began tracking healthcare cost increases.
This rising cost is not entirely beyond the control of employers and other payors, however. While a good portion of a family's typical $18,000 in medical costs is devoted to necessary treatment, an excess of 25% of total healthcare spending, or more than $600 billion a year, 2 goes toward inefficiency and waste. Minimizing this inefficiency and waste can be done while simultaneously improving quality,3 and therein lies the opportunity for employers. Employers that understand proper utilization can identify the waste and inefficiency in their own plans and thereby begin to moderate the cost of health benefits by holding their health plans and other vendors accountable for meeting reasonable utilization targets, as opposed to shifting costs to employees as do many common "cost control" techniques.
Recent efforts at cost control have yielded middling results
In recent years, plan sponsors have tried to hold down healthcare costs through a number of approaches. Many instituted disease management programs, with disappointing results. More recently, a large number of companies established wellness programs in an attempt to improve employee health and stave off the cost of more expensive procedures over the long term. But, again, these efforts resulted in a generally unsatisfactory return on investment. 4 With healthcare costs continuing to rise in the midst of the recession, a growing number of plan sponsors turned to cost-shifting to employees.5 As costs continue to rise, this approach is likely to prove unsustainable.
The challenge to all of these cost-cutting approaches is that they do not improve efficiency and reduce waste in healthcare plans. They do not take into account the flawed incentives in a fee-for-service model, which currently do not reward efficiency, quality, or adherence to best medical practices. In the current system, each service or unit of care—a doctor visit, a night in a hospital bed, a prescription drug—has a price. In employer-sponsored insurance, these unit prices are established in negotiations between physicians, hospitals, and pharmaceutical companies on one side and payors, often plan sponsors, on the other. Services are then delivered to plan members with reimbursement based on the negotiated unit prices. The utilization of these services—the volume of services provided and the composition or mix of those services—is a major source of cost variation. This variation was first made famous by researchers at Dartmouth6 and has been expounded upon in healthcare and mainstream press7 in the 20 years since.
None of these cost-cutting approaches have succeeded in improving efficiency or reducing waste in healthcare plans. As already mentioned, the average 2010 healthcare costs nationwide for the typical family of four amount to more than $18,000. However, if that family lives in Miami, New York, or Chicago, their costs will exceed $20,000, with Miami again checking in as the most expensive city at $22,089. Meanwhile in Phoenix, the family faces healthcare costs of $16,071, representing a cost difference of $6,000 (37% of the Phoenix cost) between two U.S. cities. A number of factors, such as differences in rent and physician fees, can contribute to some differences in healthcare costs, but significant variations in utilization underlie differences of this magnitude.
A better cure: Utilization management
In our fee-for-services system, payors have the clearest incentives for understanding utilization trends and how these relate to the delivery of efficient, quality care. While this previously has proven challenging, we now have the technology and empirical data about plan utilization to conduct highly informative benchmarking studies. These studies can identify areas for improved utilization, waste reduction, and better adherence to evidence-based medical practices to reduce costs and improve quality. Plan sponsors can then have an informed discussion with health plans about targeted programs to reduce unnecessary utilization and possible performance guarantees that the plans will be accountable to meet.
As an example, in a recent study we analyzed a company's active employee healthcare benefit experience to identify program areas that were performing well and those that were performing poorly. We compared its program experience with benchmarks that reflect the company's demographic profile, geographic profile, and benefit designs, using benchmarks for "loosely managed" and "well-managed" plans. Loosely managed benchmarks represented plans that have some utilization review, preauthorization, and case management that were ineffective at reducing utilization. We expected any moderately managed healthcare benefit program to produce results significantly better than these benchmarks.
Well-managed benchmarks represented nationwide claim cost and utilization targets in a highly effective managed care environment (such as a staff model HMO or a globally capitated provider group without fee-for-service incentives) that effectively applies utilization management principles across the entire continuum of medical care. This includes inpatient care, outpatient facility care, ancillary testing, routine office care, referral physician care, and prescription drugs. In the current healthcare benefit system, it may not be realistic for a given group healthcare benefit insurer or administrator to produce results equal to, or better than, the well-managed benchmarks. However, the most efficient managed care organizations produce results similar to these benchmarks. In this study, we assumed provider reimbursement levels were identical for loosely and well-managed benchmarks to focus on utilization.
An analysis of a sample employer
When we compared the company’s per member per year (PMPY) claim costs, we found they fell well above the well-managed plan and just 5% below the loosely managed benchmark.

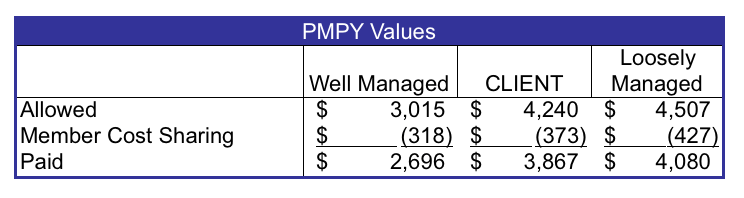
We then compared key utilization metrics for the company's subpopulation to well-managed benchmarks. As opposed to unit costs, which are determined primarily through healthcare benefit plans and provider negotiations, utilization is primarily managed by healthcare benefit plans, supplemental vendors, or both. We noted a number of areas for improvement.
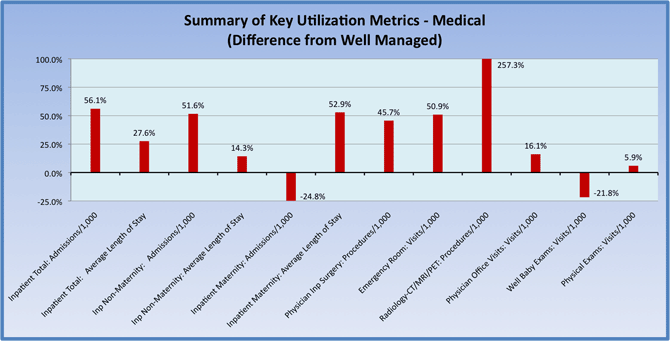
For instance, the radiology-CT/MRI/PET utilization rate shown in the above figure is significantly higher than the well-managed benchmark, and this finding was consistent with many other recent studies of radiological services. We believe the substantial increase is correlated with the increasing number of physician groups that own imaging facilities, and it is likely that advanced services are being overprescribed.
In isolation, radiology represents a small percentage of total healthcare costs. However, it has recently been a major contributor to healthcare cost trend. Additionally, overutilization of radiology services can lead to adverse side effects and indirectly increase other healthcare costs by leading to other tests and procedures that are not considered to be best practices.
In this study, we also noted the hospital non-maternity admission rate is significantly higher than the well-managed benchmark. The average non-maternity length of stay is moderately higher than the well-managed benchmark, and the physician inpatient surgery rate is significantly higher than the well-managed benchmark. The relatively high rate of emergency room utilization could be indicative of overuse of costly hospital services. This is often due to access problems for primary care services or benefit design issues. Many emergency room services can be provided at a less intensive, and less costly, setting such as an urgent care clinic, a primary care physician (PCP) office visit, or even a retail clinic.
In addition, office visit rates were significantly higher than the well-managed benchmark. There is little consensus as to the value of regular PCP visits and physicals. Certainly, an appropriate PCP visit is preferable to a specialist visit. But the value of physical exams for people without health risks or with generally healthy profiles may be negative. Physical exams have the potential to provide a false positive result or to lead to unnecessary treatment.
For this study, the company also was able to identify the impact of preference-sensitive admissions on its healthcare plan. These are procedures in which patient choice is the primary driver of the decision to have or not have a procedure or treatment. The study demonstrated an opportunity to decrease preference-sensitive admissions, which would likely entail providing patients with sufficient and unbiased information on the risks and benefits of various treatment options.
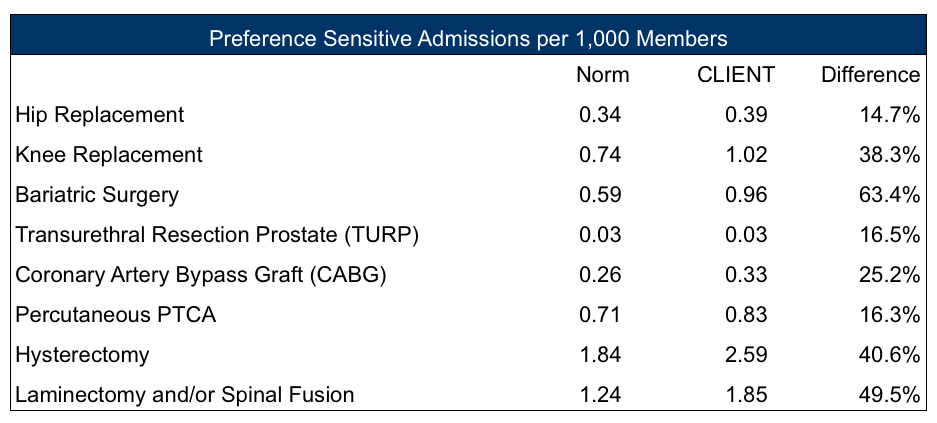
Overall, this study of an employer's utilization pointed to a number of opportunities to improve plan utilization and reduce waste, which we define as unnecessary, redundant, or ineffective treatment (and the costs associated with such treatment) that is contrary to, or not demonstrably associated with, positive healthcare quality and outcomes. Results from this type of study can be used by plan sponsors to have an informed discussion with their health plan vendors to develop reasonable targets for the next plan year and potential targets for the following two years. For this company, and all plan sponsors, working to eliminate waste in their healthcare plans will more effectively help enable efficient care delivery, reduce costs, and improve quality.
With our ongoing national debate on the healthcare system and its focus on insurance coverage, it is imperative for employers to develop and implement plans to better manage their healthcare benefit program costs without further shifting costs to employees. By means of better tools to analyze the performance of individual healthcare plans, the time is right to push through barriers for improving utilization levels and instituting tighter cost controls. Plan sponsors have the opportunity to take what has been learned from years of experience by well-managed healthcare plans and use it to better manage their own plans.
These resources were used to analyze an employer's claim experience and create benchmarks:
Milliman's Health Cost Guidelines – Commercial Rating Structures (HCGs) and Health Cost Guidelines – Prescription Drug Rating Manual. The HCGs are developed by Milliman health actuaries and represent a combination of their experience, research, and judgment. Data reflecting medical claims experience for 17 million lives and inpatient admissions data representing 75% of total U.S. admissions is used in developing the HCGs.
Milliman's Hospital Efficiency Index (HEI™) uses a highly refined statistical process to develop best-practice benchmarks for acute inpatient hospital services. The HEI best-practice benchmarks reflect actual hospital practice and not a hypothetical or "ideal" scenario. Actual hospital data for admissions and length of stay is compared on a severity-adjusted basis to the benchmarks, and variances are reported as potentially avoidable admissions and potentially avoidable days.
Chronic Condition Hierarchical Groups (CCHGs) are a new and innovative way of analyzing healthcare utilization and costs. The CCHG system is designed to organize and report medical utilization and cost in a "clinically relevant" manner and is referred to as a "clinically relevant" grouper. A constant complaint by doctors about systems used to report utilization and cost is that the reporting is not aligned with how doctors make clinical decisions about patients. CCHGs assign patients to unique categories using a clinically relevant hierarchy that groups similar patients in the same group based on how doctors make treatment decisions. This makes it easy to identify the impact of specific diseases on cost and utilization.
1 /-/media/Milliman/importedfiles/uploadedFiles/insight/Periodicals/mmi/milliman-medical-index-2010.ashx
2 /-/perspective/healthreform/transforming-healthcare-identifying-failures-insight05-01-09.php
3 /-/perspective/healthreform/pdfs/convergence-quality-efficiency-role-RR06-01-09.pdf
4 /-/expertise/healthcare/publications/published/taking-stock-of-wellness-PA04-01-8.php
5 https://www.milliman.com/en/insight/2009-milliman-medical-index
6 http://www.dartmouthatlas.org/
7 http://www.newyorker.com/reporting/2009/06/01/090601fa_fact_gawande