Introduction
The healthcare marketplace is rapidly changing. The emergence of Alternative Payment Models (APMs) requires healthcare providers to develop expertise in areas where many of them currently have little experience. A great deal of risk is being introduced into a system that is currently not well positioned to bear and manage multidimensional risk. This includes risk of underpayment, uncertainty in future payment streams, and retrospective payment adjustments among other risks. These risks along with additional APM demands have increased the need for actuarial, analytic, and data mining skills to the point that these capabilities are now required to be successful. Careful thought is necessary before contractual commitments are made, and existing capabilities most likely need to be augmented with expertise in new areas either by direct hiring or outsourcing.
CMS is driving forward
In the public insurance markets, the Centers for Medicare and Medicaid Services (CMS) has set a goal of tying 30% of traditional Medicare payments to quality or value through APMs, such as accountable care organizations (ACOs) or bundled payment arrangements, by the end of 2016. They also plan on reaching 50% of payments to these models by the end of 2018. CMS announced earlier this year that it has already met the 30% threshold ahead of schedule. Similarly, the major commercial insurance carriers have set goals similar to CMS.
CMS recently released the proposed regulations for the Merit-Based Incentive Payment System (MIPS) and the Alternative Payment Models (APMs) programs. These regulations introduce significant change for reimbursement structure (and potentially magnitude) for most clinicians under traditional Medicare. Beginning in 2017, clinicians will be evaluated based on quality, resource use, clinical practice improvement, and meaningful use of certified electronic health record (EHR) technology which will affect their reimbursement for the 2019 payment year. How they perform in these four areas can change their reimbursements between -4% to up to +12% in the first year, and go to -9% to up to +27% within four years—with some additional upside potential as well. Providers who more aggressively embrace movement toward value-based reimbursement and are accountable for the overall cost of care for their patients by participating in advanced APMs will avoid both the infrastructure demands and financial uncertainty associated with MIPS and, in addition, be guaranteed 5% bonus payments.
For hospitals, there are also significant changes to reimbursement both through changes in the calculation of the standard diagnosis-related group (DRG) payments as well as the introduction of bundled payment methods that put hospitals at risk for full episodes of care, including costs incurred after patients have been discharged from the facility. Beginning in April 2016, Medicare introduced the Comprehensive Care for Joint Replacement (CJR) program, which is mandatory for designated hospitals. These hospitals are being evaluated based on the cost and quality of care provided for patients who undergo joint replacement surgery, and it includes most Part A and Part B medical claims that are incurred for three days prior to 90 days post-surgery. After the first year of the program, hospitals will share in either the gain or loss of the cost of the CJR episode based on how they perform relative to the targets set for them by CMS.
These programs are just a sample of the shift in reimbursement and additional risk that is being placed on healthcare providers. Many other programs, both voluntary and mandatory, are in place or being introduced by both CMS and private payers. To be successful in this new environment requires new skills and new processes to improve the delivery of healthcare. Several of these required skills are in areas that have not traditionally been managed by healthcare providers. Initially, it may be prudent to look for external experts to create a plan and help build the necessary infrastructure.
Contracting
There are many contracting choices offered to clinicians and facilities by both CMS and private payers. Knowing which option at which negotiated rate will work best for them is essential to the survival and prosperity of providers. In addition, ensuring that the contract includes certain types of protection to control risk is critically important and requires forethought and planning. It would be prudent for providers to engage actuaries who possess a deep understanding of actuarial risk to assist in structuring and negotiating these risks. In addition, the reconciliation of payments from these contracts will also require analytic and actuarial resources to ensure all aspects of the contract have been properly applied.
Analytics
Advanced analytics and data management is another area that requires additional focus in order to be successful. Providers need to have a data analytic strategy with tools and resources to develop a quantitative-based plan of action that focuses clinical resources on the areas of highest importance.
A first step in this process is to complete a review of current capabilities and a gap analysis. This expertise should include capabilities in medical cost and trend analytics, population health, quality analytics, and risk score analytics (see Figure 1). In addition, development of a data warehouse and the necessary analytic tools and reporting functions will set the organization on a path to success.
Figure 1: Provider Analytic Needs
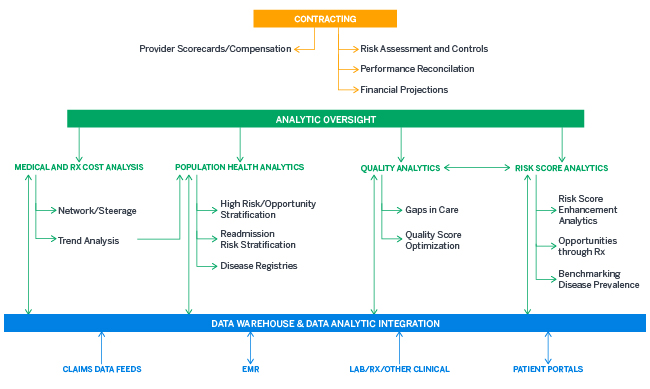
Call to action
Value-based reimbursement is here to stay and it will continue to expand and evolve. Providers need a clear strategy and action plan to address existing shortfalls and future developments. The following are steps that should be taken to ensure success:
1. Determine the right programs and contracts to participate in based on current capabilities and ability to assume risk. Assess each opportunity to ensure that adequate protection is provided to mitigate financial risk. Consider hiring qualified external resources such as actuaries to assist in evaluation.
2. Complete a review of current operational and analytic capabilities and identify gaps.
3. Create an action plan based on the gap assessment that prioritizes the areas of highest potential financial benefit. Consider hiring qualified external resources to develop and execute an action plan until internal resources are adequately staffed with necessary skills, capabilities, and capacity.
Having a strong partner with the necessary skills, experience, and knowledge can be one of the keys to ensure providers do not assume unnecessary risks and potential losses. If the appropriate resources are engaged, value-based reimbursement contracting and payment can lead to long-term success.
For more information about the material in this article, please contact Steve Kaczmarek.