The Medicare Access and CHIP Reauthorization Act (MACRA) makes significant changes to the Medicare payment system by introducing a quality-based payment model. MACRA changes how providers caring for Original Medicare members are reimbursed and includes incentives for risk-based payments by all types of payers. While MACRA primarily affects Part B clinicians, there are numerous implications, synergies, and opportunities for Medicare Advantage (MA) plans. The key questions for MA plans to consider include:
- How will MACRA affect MA plans’ provider payments?
- What synergies exist between MACRA’s quality scoring and the MA Stars quality program?
- How can MA plans help providers achieve Qualifying Participant (QP) status?
- What incentives exist under MACRA for providers to improve risk score coding?
- How are MA plans in the market responding to MACRA?
In this paper, we explore the answers to some of these questions.
Background
Medicare-eligible members today receive their benefits in one of two ways:
1. Original Medicare, where physicians contract directly with the federal government to receive compensation for care to enrollees
2. Medicare Advantage, where a private insurer acts as an intermediary between the member and the government and between the provider and the government
Figure 1 shows the breakdown of 2015 Medicare expenditures by program and risk-sharing model. Original Medicare accounted for 59% of expenditures in 2015 (of which 69% are fee for service [FFS] and 31% are tied to alternative payment methods), while MA accounts for approximately 41%.1
Figure 1 – 2015 Medicare expenditures
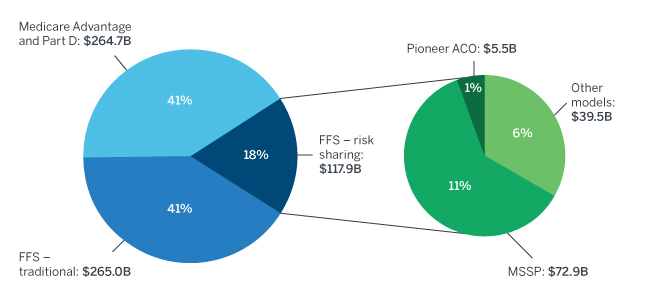
Medicare beneficiaries in Original Medicare can obtain care from most providers who then receive a payment directly from the Centers for Medicare and Medicaid Services (CMS) under a FFS arrangement. Until recently, FFS payments were not significantly adjusted for care quality or outcomes.
Currently, MA plans have significant flexibility in structuring provider contracts, benefits plans, and provider networks. This includes the ability to negotiate contracts as well as design benefit plans which steer members toward specific providers. These contracts utilize FFS reimbursement, risk-sharing contracts (both upside-only and two-sided models), or global capitation arrangements. While there is continued movement towards risk-based contracts and capitation, MA contracts are largely based on FFS reimbursement, and in particular, a percentage of Medicare FFS reimbursement.
MACRA effects on Original Medicare
Major changes brought about by MACRA include:
- Adjusted reimbursement for Part B providers. Beginning in 2019, many Part B providers will be subject to the Merit-Based Incentive Payment System (MIPS). MIPS payment adjustments2 can be positive, flat, or negative depending on the providers’ relative performance on metrics relating to cost, quality, the use of electronic health records (EHR), and clinical improvement activities.
- Bonus for qualifying participants: Some Part B providers may achieve Qualifying Participant (QP) status3 and would receive a 5% bonus to their Part B payments (in lieu of the MIPS adjustment). Providers attain QP status through substantial participation in Advanced Alternative Payment Models (Advanced APMs).
- Advanced APMs. MACRA establishes guidelines for qualification as an Advanced APM.4 Advanced APMs are defined by substantial use of certified EHRs, payments tied to quality standards, and acceptance of more than nominal financial risk.
- Part B fee schedules will be flat for multiple years. For 2020 through 2025, overall Medicare Part B reimbursement will not increase. Annual increases to the Medicare fee schedule will resume in 2026, but they will be lower for MIPS-eligible clinicians who do not achieve QP status (0.25% for MIPS-eligible versus 0.75% for QP). Additionally, the scheduled reimbursement increases between 2016 and 2019 are limited to 0.5% per year and were less than 0.5% in both 2016 and 2017.
- Encouragement toward Advanced APMs. Many of the MACRA provisions encourage providers to participate in Advanced APMs.
- Impact of quality scoring: Ultimately, all physician reimbursement will be affected by quality scoring because both MIPS-eligible clinicians and Advanced APMs receive payments that are adjusted by quality metrics.
Qualifying Participant (QP) status–effects for MA plans and providers
From the perspective of MA plans, one of MACRA’s key effects will be the push for providers to achieve QP status. From the provider’s point of view, QP status would be favorable because QPs will receive a flat 5% bonus on Part B reimbursement and avoid the potential MIPS penalties. MA and commercial reimbursement arrangements are already gradually moving toward risk sharing, and MACRA is likely to accelerate this trend by providing added incentives for providers to enter risk-sharing agreements.
For the first two years of MACRA (performance years 2017 and 2018), the definition of an Advanced APM includes only a few types of entities, including some of the Medicare Shared Savings Program (MSSP) tracks (Tracks 2 and 3 in 2017 and Tracks 1+, 2, and 3 in 2018) and Next Generation ACOs (NextGens). Participating in Advanced APMs generally involves significant infrastructure investment to manage care and quality reports in addition to the financial capacity to withstand the potential downside risks. Consequently, few providers currently qualify as participating in Advanced APMs, and many APM participants remain in programs without downside risk (e.g., 86.5% of 2017 MSSP participants are in Track 1).5
Beginning in performance year 2019 (which affects payments in 2021), CMS will introduce the “All-Payer” option for achieving QP status. Providers may then use risk-based payments from both Medicare Part B and other payers to meet the QP threshold. Because many providers are already developing or are involved in commercial, Medicare, and Medicaid risk-sharing arrangements, the inclusion of these programs in the Advanced APM thresholds will help more organizations qualify for QP status.
Synergizing quality metrics between MIPS, ACOs, and MA Stars
Many quality measures from MIPS, the MSSP and Next Gen ACOs (some of which qualify as Advanced APMs), and the Medicare Advantage Stars programs are similar or identical. By targeting a common subset of these measures, providers can benefit under all three programs, especially as Medicare Advantage contracts move toward quality-based risk contracts under the emerging MACRA All-Payer ACO paradigm.6 Figure 2 shows the weights of the Medicare Advantage Part C Star measures that overlap with MSSP/NextGen ACO and MIPS measures.
Figure 2 – Overlap of quality metrics between Medicare Advantage, MSSP/NextGen, and MIPS7
| Program | Stars weight | Percentage |
| Star measures - Part C overall | 51.0 | |
| Star measures - Part C excluding the Health Plan Quality Improvement Factor | 46.0 | 100% |
| Next Generation ACO | 20.5 | 45% |
| Medicare Shared Saving Program (MSSP) | 20.5 | 45% |
| MIPS | 30.0 | 65% |
The MA Stars program and the MSSP and Next Gen ACO programs have a fixed set of quality measures that overlap significantly. Therefore, providers who participate in Advanced APMs and also contract with MA plans have consistent incentives to improve their quality performance for both MA and original FFS beneficiaries. Recognizing these significant overlaps, and the infrastructure and capital providers need to participate in Advanced APMs, some MA plans are partnering with providers to support participation in Advanced APMs.
Under MIPS, most providers will be required to submit at least six quality measures.8 However, providers have hundreds of measures to choose from, so MA plans will need to steer providers towards the measures that benefit both parties. Ultimately, this will allow both providers and MA plans to benefit from improved quality scores under their respective programs.
MACRA effects on MA contracts
Beginning with performance year 2019, CMS’ “All-Payer” criterion allows for inclusion of provider-payer contracts from commercial, Medicare, and Medicaid arenas in the calculation of a provider’s QP status. MACRA does not require MA providers to enter into risk-based contracts or participate in quality measurement; however, more providers may seek risk-based contracts with MA plans that satisfy the Advanced APM criteria.
Entering contracts or modifying existing contracts so that they meet the definition of an Advanced APM may require significant investment by MA plans in systems and administration, especially in relation to contracting, quality measurement, and financial settlements. An Advanced APM often also requires substantial investment from providers to set up the data analytics, EHR system, and other infrastructure required to support the risk contract. In order to qualify as an Advanced APM, the contract must meet standards relating to Electronic Health Records (EHR) usage, quality metrics, and the amount of risk providers assume. Specifically,
- EHR. The APM must require participants to use certified EHR technology.
- Quality. The APM must provide for payment for covered professional services based on quality measures comparable to those in the quality performance category under MIPS.
- Nominal risk. In an Advanced APM, providers must assume at least “nominal risk.” Nominal risk is defined using either a revenue- or expenditure-based metric. Under the revenue-based metric, providers must be at risk for at least 8% of expected revenues, while the expenditure-based alternative requires providers be at risk for at least 3% of total expenditures for aligned beneficiaries.
The All-Payer model may incentivize providers to work under contracts that qualify as an Advanced APM. Advanced APMs require sophisticated cost and quality measurement, consistent with the capabilities required to be at least a 4-Star Medicare Advantage plan. As the program matures, the requirements for being considered a QP become stricter and the thresholds for Advanced APM-based patient populations or payments become higher. This may drive additional providers to seek Advanced APM-style contracts with MA plans. Risk-based contracts could be seen as a benefit to MA plans because they incentivize quality and cost containment (potentially increasing MA revenues and lowering costs), but this benefit must be weighed against the potential costs of developing, maintaining, and administering these contracts.
MACRA, MA, and Medicare fee schedules
Under MACRA, MA plans will continue to have significant latitude in how they structure contracts with physicians and provider organizations. However, because MACRA makes significant changes to Part B providers’ FFS reimbursement levels, even MA plans that continue to contract primarily using FFS will need to adapt to MACRA’s changes.
As the MACRA-based changes come into effect, the traditional meaning of Medicare FFS—which is the basis of many MA contracts—becomes much more fluid and complex. At a minimum, the definition of “Medicare FFS payment rates” will need to be clarified within provider contracts to reflect the inclusion or exclusion of MACRA/MIPS bonus or penalty payments. Successful MIPS participants and QPs may push to see the 5% bonus incorporated into their MA contracts, while lower-performing providers may not want their contracts to be adjusted to reflect MIPS’ negative effects. MA organizations will need to plan ahead and review and update contract language as well as strategize regarding the organization’s goals to avoid any potential unintended consequences of MACRA’s adjustment to provider reimbursement.
Another consideration is that, in aggregate, Part B fee schedules will be flat from 2020 through 2025, which will put increasing pressure on Part B providers. Currently, multi-year contracts between MA plans and providers may be based on a percentage of the Medicare fee schedule. In an era where the Medicare fee schedule does not increase, providers may push for contract changes.
A third area to consider for many MA plans is the rules around related parties. Related party relationships are described in MA bid rules, and generally occur where hospitals or provider groups have an ownership in MA plans. As a part of MA bid development requirements, CMS stipulates contract comparison methods in which payment levels in related party agreements are compared to payment levels in agreements with non-related parties or Medicare FFS rates. The inclusion or exclusion of MACRA-related bonuses in various contracts could have a substantial impact on the comparison result. This example highlights another area of uncertainty as the CMS rules regarding MA plans, MSSP and NextGen ACOs, and MIPS providers may need to change based on the new world of MACRA.
Conclusion
MACRA has far-reaching implications affecting Part B clinicians, MA plans, and other types of providers. MACRA presents many opportunities for health plans as provider payments move towards quality adjustments and risk sharing. Provider risk sharing may be advantageous to MA plans by incentivizing care management and quality improvement. It is important for health plan and provider leaders to understand MACRA's multi-year effects and be proactive in planning for the future.
While there is a concerted push in healthcare to implement quality and cost controls, these initiatives are complex and can require careful analysis to avoid unwanted consequences. As relationships between providers and MA payers evolve, they will have to work closely together to ensure a fair balance of risks and rewards. Because MACRA is complex and new, the potential effects are still emerging, and there are still many unanswered questions about its interrelated impacts. MA plans need to think strategically about how to respond to these changes and opportunities.
1 http://wayback.archive-it.org/3926/20170128195431/https://www.hhs.gov/about/news/2016/03/03/hhs-reaches-goal-tying-30-percent-medicare-payments-quality-ahead-schedule.html, https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/ReportsTrustFunds/Downloads/TR2016.pdf, https://data.cms.gov/ACO/Medicare-Shared-Savings-Program-Accountable-Care-O/x8va-z7cu, and https://innovation.cms.gov/Files/x/pioneeraco-fncl-py4.pdf.
2 http://www.milliman.com/insight/2016/MIPS-adjustment-overview/.
3 http://www.milliman.com/insight/2016/Challenges-and-opportunities-with-obtaining-Qualifying-APM-Participant-status/.
4 http://www.milliman.com/insight/2016/Advanced-APMs-and-Qualifying-APM-Participant-status/.
52017 Medicare Shared Savings Program Participants. Retrieved 2/6/2017 from https://data.cms.gov/ACO/2017-Medicare-Shared-Savings-Program-Participants/futz-eezk.
6 http://www.milliman.com/insight/2016/Advanced-APMs-and-Qualifying-APM-Participant-status/ and http://www.milliman.com/insight/2016/Challenges-and-opportunities-with-obtaining-Qualifying-APM-Participant-status/.
7Based on internal analysis. In some cases, measures are not identical but largely the same, such as using a different age range. Sources:
2016 star rating technical notes: https://www.cms.gov/medicare/prescription-drug-coverage/prescriptiondrugcovgenin/downloads/2016-Technical-Notes-Preview-1-v2015_08_05.pdf
Next Generation ACO request for applications: https://innovation.cms.gov/Files/x/nextgenacorfa.pdf
2016 MSSP quality benchmarks: https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/sharedsavingsprogram/Downloads/MSSP-QM-Benchmarks-2016.pdf
MIPS quality measures: https://qpp.cms.gov/measures/quality.
8 http://www.milliman.com/insight/2016/MIPS-adjustment-overview/.