Pharmaceutical prices and the purpose of pharmacy benefit managers (PBMs) received no shortage of attention in recent months, especially in light of both congressional and White House pressure to tackle the high cost of prescription drugs. The complex business model—one that, by nearly all accounts, is lacking in transparency—came about out of necessity from the increased and overwhelming complexity of pharmacy claims processing.1 However, where there is complexity and unequal access to information, there is often room for increased efficiencies and opportunities for disruption.
The pharmaceutical industry has many stakeholders. The primary purpose of the PBM is to serve as an intermediary among pharmacies, drug manufacturers, and payers. PBMs manage formularies, negotiate discounts and rebates, and process and pay prescription drug claims through a web of electronic transactions.
Blockchain could potentially transform the relationship between payers, pharmaceutical manufacturers, wholesalers, and pharmacies by offering an alternative, transparent mechanism for processing, pricing, and validating prescription transactions. This approach could lead to less waste, reduced pricing variations between pharmacies, and a better app-based purchasing experience for consumers, through transparency of the true cost of prescription drugs.
This article describes: 1) the origin of PBMs; 2) how claims are processed; and 3) ways in which blockchain could disrupt the PBM marketplace. The article does not address every aspect of blockchain, but rather is intended to start a conversation about the potential for disruption of this emerging technology.
Bear in mind, the pharmacy benefit space has many niches. The content of this paper may apply to state and federal health plans, but the focus of this paper is on the private healthcare space.
The origin of PBMs
PBMs as we know them today originated during the early 1980s when the health insurance and pharmaceutical market grew rapidly in size and complexity because of technological advancements. As the demand for prescription drugs increased, pharmacists and insurance companies found themselves overwhelmed manually processing claims. The need for an intermediary to adjudicate prescription claims arose and PBMs developed to fill that gap. PBMs served as financial intermediaries, negotiating lower prices with the drug manufacturers. They also promised to make processing of prescription claims easier and more efficient.2
The growth of PBMs during the 1980s and 1990s created a web of contracting complexities which eventually shielded patients from the actual cost of prescriptions. Utilization and prices subsequently grew at an outstanding rate. Patients struggled to make cost-based purchasing decisions and there was no mechanism to exert market pressure on manufacturers and PBMs.
Then the Medicare Modernization Act of 2003 provided a significant boost to the PBM industry. As Medicare Part D expanded to cover prescription costs, PBMs found themselves playing a significant role. To reduce the administrative burden on insurance companies, PBMs assumed the role of identifying patients eligible for Medicare Part D as well as setting drug prices with manufacturers through discounts and rebates.
In this role, PBMs set the formulary. If a drug was not on the formulary, doctors would be less likely to prescribe it and insurers would not cover the cost. This gave the PBMs tremendous power to negotiate prices with drug manufacturers and shield consumers for the actual cost of medications. Today, there are less than 30 mid-to-large PBMs, with three major PBM companies (CVS, OptumRx, and Express Scripts) handling between 70% and 75% of the prescription claims.3 All three of the largest PBMs own or are controlled by a major health plan.
How PBMs currently process and store prescription drug claims
PBMs currently use a traditional database management system (DBMS) model to adjudicate and store prescription claim data. A DBMS allows users to create and manage one or more databases. A traditional DBMS is based on a centralized client/server model, where clients communicate with a centralized server where data is stored. A simplified example of this is the way many businesses have computers for each employee, but store the company’s data in a centralized server facility. Users must be authenticated before they can view and edit the data and users with enough authority can create, read, update, and delete data in a traditional client/server DBMS model. If the security on a database is compromised, a malicious user can modify, corrupt, or even delete information on a database. Additionally, the direct availability of the data to mutual third parties is generally discouraged due to security concerns.
Figure 1: Centralized DBMS approach
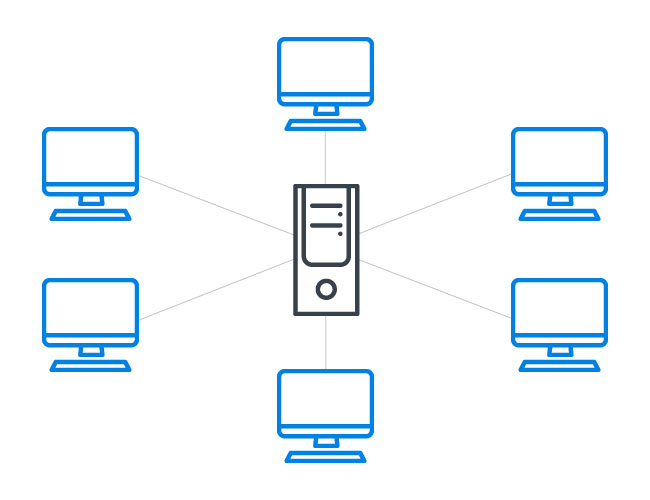
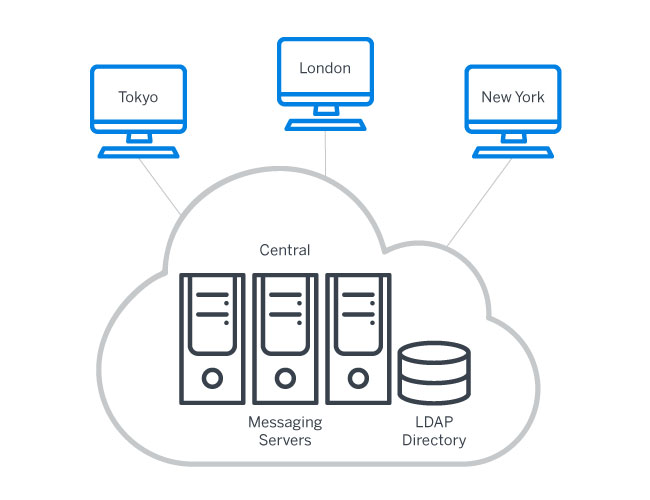
Figure 2: Cloud-based DBMS
Blockchain DBMS model
Blockchain is an emerging technology that is often designed to offer a distributed ledger system to accurately validate and confirm transactions. In common configurations, each participant has access to a copy of the ledger databases. Various consensus algorithms can be utilized to make it very difficult to change the ledger history. Data that cannot be changed is called immutable, one of the most desirable characteristics in blockchain. One way to explain the concept is the “glass safe” analogy, originally coined by Fabricio Santos of Cointelegraph: imagine a bank vault filled with glass safe deposit boxes in which participants can view the contents of all the boxes but cannot access them. When a person opens a new deposit box, that person receives a unique key to that box but does not own the box—only the contents inside it. Because all box owners can see the contents of each box, the group can validate them, but individuals can access only their own.4
It is a common misconception that everyone can see everything on a blockchain. For a fully public blockchain, like cryptocurrencies, this is partially true. Everyone can see the first blockchain transaction ever posted, the most recent, and everything in between. The transaction itself is visible, but the real-world identity of the individuals and entities behind the transactions remain hidden. As blockchain emerges in private enterprises, it will not be open to everyone. Private blockchain designs might be a practical solution for some business problems. A drug manufacturer, for example, may participate in a private blockchain with its wholesaler in an effort to prevent fraud, waste, and abuse. There are even semi-private blockchain solutions. They can be implemented by a large agency, for example (like state and federal governments), allowing other large organizations (like auto manufacturers and insurance groups) to participate in an effort to improve vehicle safety.
In contrast to a traditional DBMS model, blockchain technology uses a decentralized model. Blockchain employs a series of nodes to validate transactions. To complete a transaction, a series of nodes must validate it before it is stored and digitally signed and encapsulated into a block of data. Once encapsulated, consensus algorithms can help protect a block from being altered or destroyed. As new transactions are generated, validated, and encapsulated, they are strung together to create a chain.
Properties of blockchain that make it useful are shown in the table in Figure 3.
Figure 3: Uses of blockchain
| Property | Use case | Real-world example |
| Immutability | All participants agree on the same history, reducing disputes about historical events. | The country of Georgia implemented a public blockchain for land title transactions. 5 |
| Transparency | Transparency in a marketplace leads to better decision making by all parties. | Walmart implemented blockchain in its food supply chain to track the origin of products from multiple suppliers. 6 |
| Smart contracts | Transparency is not just access to the data. Smart contracts represent transparent access to business logic. | Cryptocurrencies have reduced transfer fees imposed by banks, lowering the cost of money transfers. 7 |
DBMS and PBMs: Can blockchain disrupt the PBM market?
A traditional DBMS uses a client/server model. In contrast, a blockchain DBMS uses a decentralized model. A distributed network of nodes validates all transactions. Blockchain data is stored throughout the distributed network rather than in a centralized server. Simply put: all participants of the system (that are running a node) validate a transaction before it is committed, ensuring transparency for everyone.
The current DBMS-based ecosystem is complex, inefficient, and sometimes opaque. Relevant pharmacy claims data is stored in one centralized location (managed by the PBM), and both retail pharmacy and payer transactions must operate through that centralized database in order to process pharmacy claims. Claims that are submitted by a pharmacist for a prescription must be adjudicated and reimbursed by the PBM, which then bills the insurance company and manages the rebate process with the manufacturer. The process can take upwards of 60 days.
In a blockchain model, no centralized storage database is needed. Instead, claims transactions, like the contents of the glass safe deposit boxes, can be viewed, validated, and distributed by all stakeholders simultaneously. Such a system could fuel an entirely different consumer experience. A consumer could walk into a retail pharmacy and, using a phone or card, pay for a prescription, and have the relevant claims data, utilization, cost, and rebates all calculated concurrently at the point of sale using blockchain technology.
Specific benefits of blockchain applications include:
-
Drug pricing. Under the current system, PBMs control the drug formulary in most situations. The formulary determines which drugs the insurance company will pay for and which drugs providers can prescribe for coverage. This provides an incentive for drug manufacturers to negotiate higher rebates with PBMs in order to have their drugs included on the formulary. However, these negotiations are not transparent, and there is a lag between when prices are negotiated and when health plans and payers receive the pricing information. This approach shields the consumers for price differences, which often vary significantly for both drugs and pharmacies.
A blockchain application could enable the pricing information to be encoded into a smart contract that can then be executed at the point of sale and quickly validated by all parties. This could evolve to simplifying the pharmacy claims process to be a credit card transaction that enables the consumer to purchase products at the least expensive pharmacy in network. The pharmacy pricing information would be available online in a manner that all other consumer products are purchased by. - Efficiency. Blockchain systems use a feature called smart contracts: coding that provides conditions that must be met before a transaction can be validated and signed. Utilizing smart contracts, drug manufacturers and insurance companies could set the criteria for drug prices and coverage. Insurance companies could also instantly update information as patient coverage changed or was rescinded. Currently, when a patient goes to a doctor, a series of transactions and phone calls is initiated to update and verify insurance. When the patient presents a prescription at the pharmacy, the insurance coverage is verified again. If any of the insurance information is entered incorrectly, it may result in the PBM rejecting the claim, leading to resubmission of the claim. Many PBMs charge a fee every time they process a claim or resubmission. A blockchain system with smart contracts could apply the validations closer to the point of service, letting users iterate to an approved claim faster.
- Durability. Unlike a traditional centralized DBMS, a blockchain DBMS is decentralized, eliminating any single point of failure. Furthermore, a blockchain DBMS only permits transactions to be read or created, guaranteeing an audit trail for all transactions.
The future of PBMs and blockchain
Although blockchain technology appears to hold great promise for the PBM marketplace, there are several obstacles to overcome before that promise becomes a reality and the PBM industry is primed for an evolution.
While blockchain has demonstrated great potential for security in cryptocurrency, its true potential in healthcare has not yet been evaluated. Further testing and implementation would be required before a blockchain application could be used on a large scale in the PBM marketplace.
All members of the ecosystem—payers, providers, pharmacies, and PBMs—would need to agree on the validation and approval criteria. As we have seen in other complex capitalized industries, finding consensus among stakeholders can pose a challenge.
Conclusion
Industry stakeholders can agree the future should hold a more efficient, less complex, more transparent, and easily accessible integration of all healthcare information and technology data. Today, the electronic approach to processing pharmacy claims is still the same one used and designed back in the early 1980’s.
The current ecosystem among pharmacies, payers, providers, and PBMs is neither cost-effective nor transparent to shareholders across the pharmaceutical supply chain spectrum. It is inefficient and has resulted in patients and payers absorbing the additional cost of the complex infrastructure that has resulted in higher prices in prescription drugs.
A blockchain system could increase transparency and trust among all parties involved and increase savings to the patient. Payers and pharmacies would benefit from blockchain by reducing the time they spend validating insurance coverage, making phone calls, and managing data. PBMs and other interested parties should work to evaluate a blockchain alternative now with an eye toward a more efficient drug financing system. The more efficient system would be able to handle additional technology improvements that the next generation is prepared to adopt. This includes real-time integration of healthcare devices, user applications, medical providers, consumerism-shopping tools, and integration to non-healthcare purchases.
1Lipton, H. L., Kreling, D. H., Collins, T & Hertz, K. C. (1999). Pharmacy Benefit Management Companies: Dimensions of Performance. Retrieved June 27, 2019, from https://www.annualreviews.org/doi/full/10.1146/annurev.publhealth.20.1.361#_i4.
2Kaupp, G. S. & Lynch, S. B. (2002). To Regain Control of Drug Costs, Health Plans Must Understand the Road They've Traveled. Retrieved April 11, 2019, from https://www.medscape.com/viewarticle/432389_1.
3Yu, Nancy L., Atteberry, Preston, & Bach, Peter B. (July 31, 2018). Spending on prescription drugs in the US: Where does all the money go? Health Affairs. Retrieved June 18, 2019, from https://www.healthaffairs.org/do/10.1377/hblog20180726.670593/full/.
4Santos, Fabricio (2016). Explaining blockchain to laypeople: The analogy of the glass box. Medium. Retrieved June 18, 2019, from https://medium.com/@lunes.platform/explaining-blockchain-11695afee9c0.
5Shang, Q. & Price, A. (2018). A blockchain-based land titling project in the Republic of Georgia. Innovations. Retrieved June 18, 2019, from https://www.mitpressjournals.org/doi/pdf/10.1162/inov_a_00276.
6Unlock. Walmart Case Study on Food Supply Chain Transparency Using Blockchain. Retrieved June 18, 2019, from https://www.unlock-bc.com/news/2019-02-22/walmart-cse-study-on-food-supply-chain-transparency-using-blockchain.
7Geiregat, S. (October 2018). Cryptocurrencies Are (Smart) Contracts. Computer Law and Security Review. Retrieved June 18, 2019, from https://www.sciencedirect.com/science/article/pii/S0267364918302279.