The Patient Protection and Affordable Care Act (PPACA) introduces new restrictions on insurers’ ability to use demographic variables to price policies in the individual and small group markets. Gender, age, and other community variables have long been used for premium price differentiation. However, beginning on January 1, 2014, rates may not differ based on gender, and must adhere to a maximum 3:1 ratio when comparing the premium for the most expensive adult age group and the least expensive adult age group. These new regulations will increase the difference between healthcare costs and what insurers are allowed to charge in premiums, raising the potential for adverse selection as traditionally less expensive demographics, such as young males, seek other health insurance alternatives. Plans will also be allowed to vary rates by area, tobacco use, and family size, but those factors are unlikely to offset this effect. Although much of the recent focus on the implications of this change is on the age limitations, in reality much of the restriction’s impact is caused by moving to unisex rates.
Comparison of new underwriting restrictions to current practice
Prior to the PPACA, it was the prerogative of individual states to decide what limitations (if any) insurers would face in using gender and age as rating tools. The majority of states placed few such restrictions on their insurance markets, as the following statistics show:
- For gender rating, 36 states do not meet the PPACA regulations. Only 14 states prohibit gender rating in both their individual and small group markets.
- For age rating, 43 states do not meet the PPACA regulations. These states have either no regulations on age rating or a maximum allowed difference in age rating bands that is wider than the 3:1 ratio mandated by the PPACA.
- All told, only seven states have gender and age restrictions as tough as those mandated by the PPACA for both their individual and small group markets.1
For further details on gender and age restrictions by state prior to the PPACA, see Appendix A.
Effect of gender on claim costs in a commercial population
According to the Milliman Health Cost Guidelines™, we can see that females incur higher medical costs than males through their 50s, and that males cost more thereafter (see Figure 1). The cost gap is most noticeable at younger ages; females under the age of 35 cost twice as much as males of similar age.
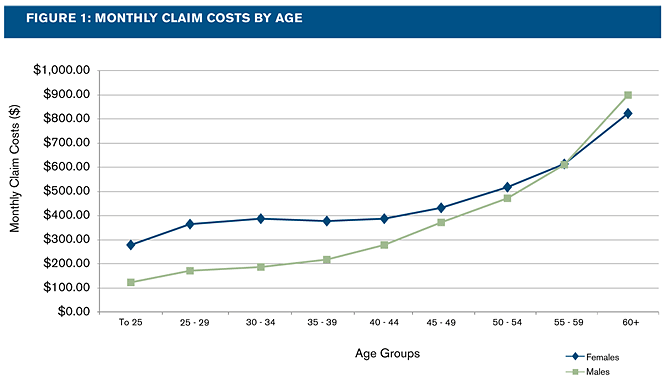
Overall, adult females cost 29% more than their male counterparts, and as a result, unisex rates allowed under the PPACA will generally result in lowered premiums for females and a corresponding increase in premiums for males.
Effect of age on claim costs in a commercial population
Although older enrollees incur more costs than younger enrollees, some of this discrepancy is mitigated by unisex rates. Men tend to have a much larger ratio between the costs of the oldest and youngest age cohorts than women.
We find that after accounting for unisex pricing, the expected claim cost ratio between the oldest and youngest adult cohorts is approximately 4.2:1 (see Figure 2 ).
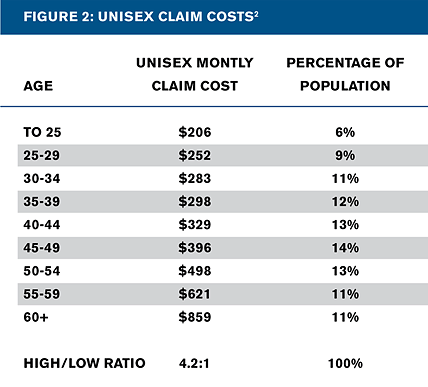
For comparison, the age cost ratio for males alone is approximately 6.7:1, and the ratio for females alone is approximately 2.9:1. Unisex pricing brings the overall age cost ratio between these two values.
In order to meet the required 3:1 age bands, one common goal is to price as many people as accurately as possible. Conceptually, this approach is accomplished by putting a floor and a cap on the age/gender factor curve, and allowing the factors within those to be unrestricted (see Figure 3). As a result, we’ve taken the youngest 6% of the population and increased their premiums by approximately 31%, the next youngest 9% of the population and increased their premiums by approximately 7%, and the oldest 11% of the population and decreased their premiums by approximately 6%.
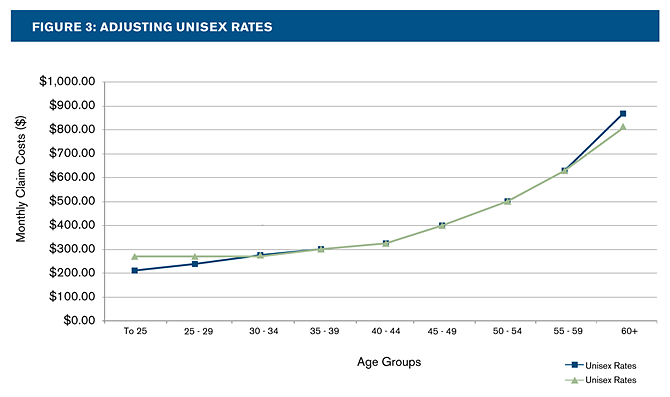
The points at which the cap and floor would be implemented to restrict the curve within the 3:1 limits should be adjusted to meet the needs of the insurer. The higher the floor is set, the higher the cap should be to maintain the 3:1 limits. When the floor is set higher, a larger portion of people at younger ages will see increases as compared to the current rates, and fewer at older ages will have reductions. The location of the floor and cap should be set to neutralize revenue and meet management goals, while being mindful of the effects of adverse selection and competitiveness. Each insurer will need to determine how to strike the right balance between attracting the youngest adults and being able to cover the costs of the oldest adults.
Insurers should also consider the impact of deductibles when implementing a 3:1 ratio. A deductible shifts some of the cost burden to the consumer such that the insurer can charge a lower premium. Deductibles do not vary by age, and the youngest and oldest age groups will pay the same dollar amount in deductibles (for those who incur costs beyond the deductible). However, the deductible represents a much larger percentage of total claim costs for individuals at younger ages. Traditionally, this has allowed high-deductible policies for young members to be priced at a low level to attract more membership. Meeting the maximum 3:1 ratio between the premiums of the oldest and the youngest age groups will likely require a relatively larger increase in the youngest members’ premiums in cases where the deductible is high. This increase in premiums would make the plans less appealing to the younger population. After 2014, insurers will need to carefully consider the premiums for high-deductible plans in order to strike the right balance between pricing products accurately and retaining/acquiring younger members in these plans.
Impacts on commercial insurance market
There is some concern about the possibility of the gender and age rating restrictions causing adverse selection. An individual mandate would serve as a barrier to low-cost members looking to leave the market entirely. However, several avenues remain through which adverse selection may occur under the PPACA as a result of the new restrictions on gender and age rating:
- Grandfathered plans: Grandfathered plans are not subject to the same gender and age restrictions as new plans in the individual market. If lower-cost individuals stay with their old plans and higher-cost individuals seek coverage under the new rating rules, the lack of lower-cost individuals in the new market will lead to higher premiums.
- Catastrophic medical plans: Even if the individual mandate provides younger, low-cost members with disincentives to leave the insurance market altogether, adverse selection can still occur if they instead migrate to catastrophic plans, which provide a limited amount of high-impact benefits and let the individual self-insure for more routine care.
- PPACA risk adjustment: The PPACA includes provisions that reimburse insurers for above-average risks they carry in the individual and small group markets. If these payments fail to accurately compensate insurers for the inherent cost differences among different ages, insurers may be wise to target low-cost populations, and any adverse selection effects from other sources will be magnified. If these payments overcompensate for above-average risks, insurers may be wise to target high-cost populations. It is unclear at this point how specifically age and gender will be considered as part of the risk-adjustment process.
The complexity of the issues above makes it challenging to predict the final effect of the PPACA’s gender and age rating restrictions on the level of premiums and overall coverage in state-based insurance exchanges. In isolation, the ban on gender rating and the 3:1 age banding may necessitate substantial changes in premiums for some members.
Appendix A
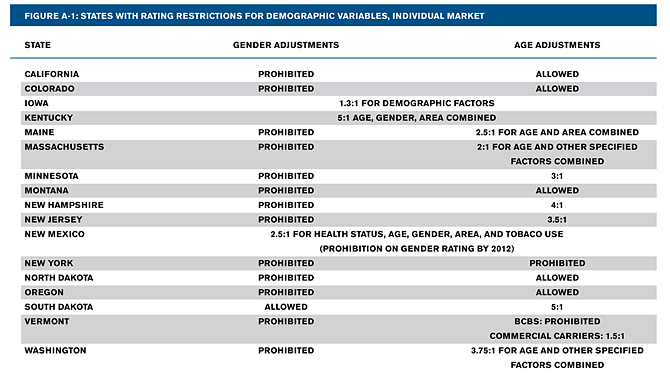
Source: “New Federal Rating Rules,” Appendix A, last modified September 22, 2010. Available at www.acscan.org/pdf/healthcare/implementation/background/NewFederalRatingRules.pdf.
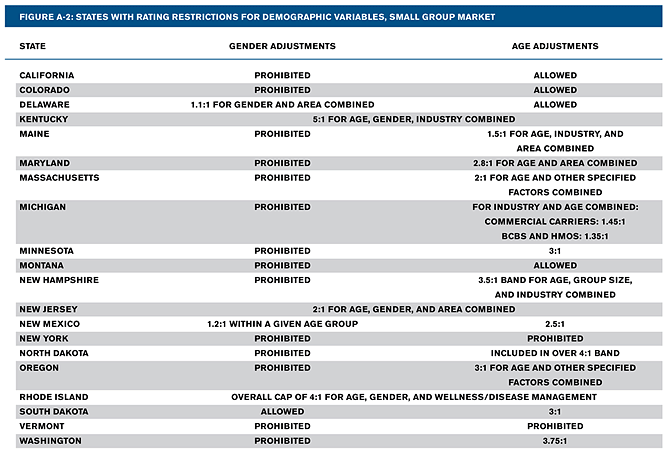
Source: “New Federal Rating Rules,” Appendix A, last modified September 22, 2010. Available at www.acscan.org/pdf/healthcare/implementation/background/NewFederalRatingRules.pdf
1 Corlette, S. (last modified Sept. 22, 2010). New Federal Rating Rules, Appendix A. American Cancer Society. Retrieved April 5, 2011, from http://www.acscan.org/pdf/healthcare/implementation/background/NewFederalRatingRules.pdf.
2 Source: Milliman Health Cost Guidelines. Claim costs represent nationwide average undiscounted billed charge levels, under a comprehensive major medical plan.