Medicaid Population Management
In previous blogs, we’ve discussed Population Management concepts and given specific examples of pediatrics, ACO, and clinical populations. In this blog we turn to the Medicaid population. Medicaid has unique characteristics because of the nature of the financing and because of the social demographics of the population served. This population is going through big changes because of Medicaid expansion and the advent of programs that may resemble some of the characteristics of Medicaid, such as subsidized rates through the federal and state exchanges.
A key to analyzing this population is to create homogeneous sub-populations. There are several ways to define the sub-populations:
- Program – CHIP, TANF/AFDC, ABD (duals), Waiver programs
- Type of delivery model – Managed Care and Fee for Service
- County – Rates are typically defined at the county level for managed care and care delivery is organized around counties
- Special populations – Pregnant women, children, mentally ill
There are specific issues that drive the metrics and analysis for Medicaid recipients, including:
- High levels of emergency department (ED) use – This population has much higher ED usage rates which often reflect access and socio-demographic issues
- Maternity – This population has higher rates of maternity and has wider variability in maternity outcomes
- Behavioral Health – Managing behavioral health is a more important component of care
- Community Resource Access – Population wellness is much more dependent on additional community resources such as case workers, food banks and social workers
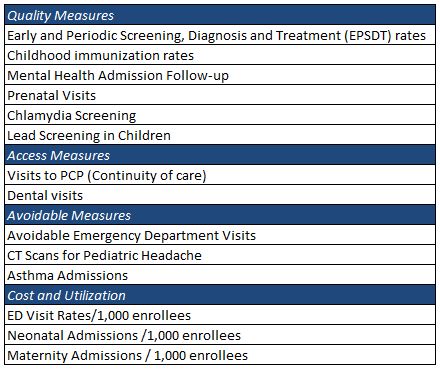
It’s important to focus on the key issues that drive the results for the population and to create metrics that reflect these key issues and characteristics. Below are some sample metrics that should be tracked and improvement goals developed.