Understanding the scale of the opioid epidemic within the insurance industry
Over 25 million American adults report suffering from chronic pain on a daily basis, and a range of adverse health outcomes accompanies their pain.
This is according to a study of 2012 National Health Interview Survey data, which also found that adults with severe pain were more likely to report taking medication for depression, feeling exhausted, nervous, or anxious every day, and were more likely to miss work for health-related reasons.1 Adults with severe pain also accessed medical care more frequently and reported having poorer health, which is associated with increased mortality.2
With the health, well-being, and daily functioning of millions of Americans on the line, our health care system has found itself walking a tightrope between crises of under-treatment and over-treatment for those who suffer from pain. Beginning in the early 2000s, opioid analgesics were increasingly seen as a solution to the problem of under-treatment that had been a concern in the 1990s.3 From 1991 to 2011, the number of opioid prescriptions filled at U.S. retail pharmacies nearly tripled, increasing from 76 million to 219 million per year, though those numbers have started to decrease since the peak in 2011 (see Figure 1).4
Despite the recent decrease in prescriptions of opioids, the human toll of the opioid crisis has continued to intensify. Illegally acquired heroin and synthetic opioids such as fentanyl have become the leading cause of overdose deaths.5 From 2000 to 2015, the rate of opioid overdose deaths increased 347% (from 3.0 deaths per 100,000 population to 10.4), with over 33,000 people dying from opioid overdoses in 2015.6 The latest data from the Centers for Disease Control and Prevention (CDC) suggests that the crisis may still be accelerating, with a 28% increase in opioid overdose deaths in just one year from 2015 to 2016.7 Opioid overdose deaths are now the single largest factor slowing the growth in U.S. life expectancy, and if current trends continue, opioid overdose deaths could outnumber suicides by 2019.8
Figure 1: Opioid prescriptions dispensed by U.S. retail pharmacies
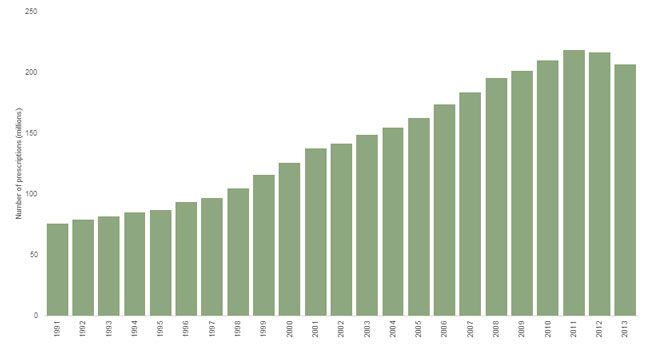
Source: IMS’s National Prescription Audit (NPA) & Vector One ®: National (VONA).
While the CDC carefully tracks opioid overdose deaths, less is known about the scale of intermediate outcomes such as diagnosed opioid use disorder. According to extrapolations from the 2014 National Survey on Drug Use and Health, 2 million Americans reported having a substance use disorder involving prescription pain relievers and 591,000 had a substance use disorder involving heroin.9
Diagnosed opioid use disorder
In order to build upon these self-reported metrics and provide a perspective on the scale of medically acknowledged opioid use disorder (meaning opioid use disorder that has been diagnosed in a healthcare setting), we have undertaken a cross-sectional study of the diagnosed prevalence of opioid abuse, dependence, or poisoning10 (hereafter referred to as opioid use disorder) within privately and publicly insured populations in the United States.
The actual prevalence of opioid use disorder may be much higher than the diagnosed prevalence rates presented throughout this report, as only a subset of those with opioid use disorder have had their disorder recognized by a medical professional. This subset is the population that health plans and providers can most readily identify and work to manage. These distinctions are further described in Figure 2.
Figure 2: Opioid use among U.S. adults in 2015
| Opioid use |
|
| Opioid use disorder |
|
| Diagnosed opioid use disorder |
|
Source: 2015 National Survey on Drug Use and Health and Milliman analysis.11
We used several large national research databases containing administrative claims data for millions of people with both Medicare and private insurance plans. We also incorporated findings from a similar analysis performed by the Kaiser Family Foundation for Medicaid beneficiaries to develop a more complete perspective on opioid use disorder across the three major insurance payers in the United States.
Based on a sample of over 42 million people with commercial insurance, nearly 1.3 million Medicare beneficiaries, and a Kaiser Family Foundation analysis of Medicaid beneficiaries in 49 states, we estimate that over 1.5 million insured Americans were diagnosed with an opioid use disorder in 2015 (the most recent year available). Figures 3 and 4 summarize these findings by payer. These results (and others presented throughout this report) have been age- and area-adjusted to be representative of the U.S. insured population as of 2015 using U.S. Census Bureau data.12
Figure 3: Diagnosed opioid use disorder by payer, 2015 (or most recent year)
| Commercial (2015) 622,000 |
Medicare (2015) 239,000 |
Medicaid (2013) 642,000 |
We found that about 41.4% of those with diagnosed opioid use disorder were commercially insured, 15.9% were Medicare beneficiaries, and 42.7% were Medicaid beneficiaries. Overall, the diagnosed prevalence rate of opioid use disorder was 3.28 per 1,000 for the commercially insured, 5.39 per 1,000 for those with Medicare, and 8.90 per 1,000 for those with Medicaid. Across all insurance payers, we found that the prevalence of opioid use disorder was 4.91 per 1,000.
Figure 4: National estimates of opioid use disorder diagnosis by payer, 2015 (or most recent year)
| Payer | Diagnosed prevalence per 1,000 | Total diagnosed nationally No. (%) |
| Commercial (2015) | 3.28 | 622,000 (41.4) |
| Medicare (2015) | 5.39 | 239,000 (15.9) |
| Medicaid (2013) | 8.90 | 642,000 (42.7) |
| Total | 4.91 | 1,503,000 (100.0) |
Opioid use disorder by age and sex
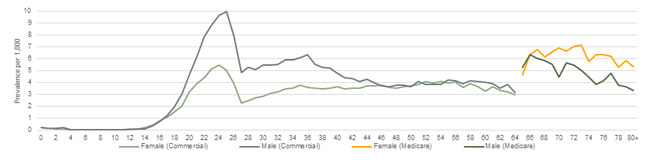
Rates of opioid use disorder varied widely by age and sex, with men generally experiencing higher rates of opioid use disorder through age 65, and women experiencing higher rates from 66 and older. Rates were quite low through childhood, followed by a marked increase in the late teen years, peaking in the mid-20s at a rate of 5.47 per 1,000 for women (at age 24) and 10.00 per 1,000 for men (at age 25). Rates showed a sharp drop-off in the late 20s, followed by a rise to another peak in the mid-30s of about 3.76 per 1,000 for women (at age 35) and 6.37 per 1,000 for men (at age 36). From the late 30s through age 64, the gap between men and women closed and both experienced prevalence rates hovering between 3.50 to 4.00 per 1,000 through retirement age. Opioid use disorder rates for Medicare beneficiaries were generally higher for women than for men, and tapered off with advancing age. Comparable data for Medicaid were not available.
The sharp decline in the prevalence rate after age 26 coincides with the expiration of dependent coverage eligibility on a parent’s plan under the Patient Protection and Affordable Care Act (ACA). We found that 87% of those diagnosed with opioid use disorder under age 26 were dependent children or young adults. Other studies have found that heroin use tends to be more common than prescription abuse for this demographic.13
Figure 5 provides the prevalence rates by age and sex, both for the commercially insured (ages 0-64) and for Medicare beneficiaries (ages 65+).
Figure 5: Diagnosed prevalence of opioid use disorder for commercial insurance (ages 0-64) and Medicare (ages 65+) by age, 2015
Variations between states
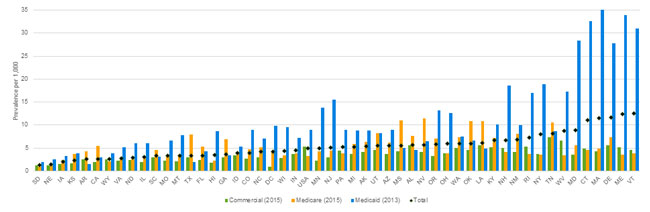
We found substantial variation between states, with a nearly tenfold difference in the diagnosed prevalence of opioid use disorder between the most and least impacted states (12.56 vs. 1.32 per 1,000 for Vermont vs. South Dakota, respectively). The most and least impacted showed an eight-fold difference for commercial insurance (7.36 vs. 0.87 per 1,000 for Tennessee vs. Washington, D.C, respectively), an 11-fold difference for Medicare (11.43 vs. 1.00 per 1,000 for Nevada vs. South Dakota, respectively), and a 22-fold difference for Medicaid (35.53 vs. 1.59 per 1,000 for Massachusetts vs. Arkansas, respectively).
Figure 6 provides prevalence rates by payer and state, as well as the overall prevalence rate across each insurance type.
Figure 6: Diagnosed prevalence of opioid use disorder by state and payer, 2015 (or most recent year)14
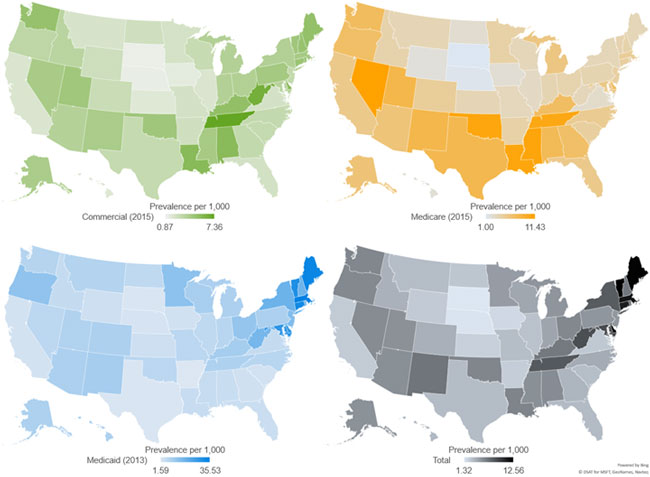
For those with commercial insurance, high opioid use disorder rates are clustered in the Appalachia region, as well as Louisiana, New England, and Washington state. For Medicaid beneficiaries, high opioid use disorder rates are heavily clustered in New England, while for Medicare beneficiaries the hardest-hit states include Nevada, Mississippi, Louisiana, Oklahoma, and Tennessee. When considering all three insurance types together, the northeastern United States is experiencing the worst of the crisis, although there is reason for significant concern across much of the country.
Figure 7 provides a heat map of opioid use disorder prevalence rates by payer.
Figure 7: Diagnosed prevalence of opioid use disorder by state and payer, 2015 (or most recent year)15
Data sources and methodology
This analysis is based on three large national research databases, as well as a prior study completed by the Kaiser Family Foundation:
- 2015 Truven MarketScan Commercial Claims and Encounters Database®
- 2015 Milliman Consolidated Health Cost GuidelinesTM Database
- 2015 Centers for Medicare and Medicaid Services (CMS) 5% Sample Standard Analytical File
- Kaiser Family Foundation analysis of 2013 Medicaid Statistical Information System and Urban Institute estimates from CMS-64 reports16
The Truven MarketScan research database reflects the healthcare experience of employees and dependents covered by the health benefit programs of large employers, health plans, and government organizations. These claims data are collected from approximately 350 payers. The MarketScan Commercial Claims and Encounters Database includes data from active employees, early retirees, COBRA continuees, and dependents insured by employer-sponsored plans.
The Milliman Consolidated Health Cost Guidelines Database contains healthcare experience primarily for large group commercial members, using data contributed from a number of payers with which Milliman has data purchase or trade agreements. Milliman collects this data from various health plans for use in product development, research, and client projects.
The CMS 5% Sample Standard Analytical File contains healthcare experience for a random 5% sample of Medicare beneficiaries across the United States.
All of the Medicaid results presented in this report are derived from a report produced by the Kaiser Family Foundation using 2012 and 2013 Medicaid data from the Medicaid Statistical Information System, which contains healthcare experience for Medicaid beneficiaries in participating states. For Rhode Island and Kansas, 2013 data were not available, so 2012 data were used instead. No data were available for Colorado. For the purpose of this analysis we have used the national average opioid use disorder rate as an estimate for Colorado’s rate.
The results presented in this report for commercial insurance and Medicare beneficiaries have been age- and area-adjusted to reflect the 2015 U.S. insured population, using U.S. Census Bureau data. The differences between crude and adjusted rates were minimal.
Next steps
Those diagnosed with opioid use disorder likely represent just a fraction of those who have problematic opioid use at any given time. Some may not fully recognize the dangers of prescription opioid abuse, while others may try to evade diagnosis out of concern for their privacy or potential legal consequences. Others may be aware of their problem opioid use but have not yet reached out for help from a medical professional.
In an upcoming report, we will explore opioid use patterns both in those diagnosed with opioid use disorder, as well as in non-diagnosed “super-users” (those who fill extraordinarily high volumes of opioid prescriptions in a year but have not been diagnosed with an opioid use disorder).
We’ll also expand on this report with some additional context on the healthcare settings that are most impacted by problem opioid use, including estimates of the direct costs of caring for those with opioid use disorder.
The opioid epidemic is a complex and growing phenomenon that needs careful study from a wide variety of perspectives in order to make progress. We look forward to contributing to this national conversation with unique analyses that combine actuarial and public health perspectives.
Caveats and limitations
The opioid epidemic has been growing at an alarming pace, and retrospective analyses will likely continue to understate the full magnitude of the problem until the tide turns and problem opioid use begins to decrease. The Medicaid results in this report are likely to be especially understated, as they pre-date the Medicaid expansion that occurred under the ACA in 2014, and because they are an additional two years older than the Medicare and commercial data. Additionally, Medicaid results were not available for Colorado, so national rates were used as an estimate. The actual rate in Colorado likely differs from this estimation.
The commercial results largely reflect large group, employer-sponsored insurance, and thus likely under-represent lower-income households that purchased individual coverage under the ACA. Additionally, while sampling errors are quite small due to the large sample sizes available in each data set used for this analysis, sampling bias could be present to the extent that health plans and payers that contribute to the research databases differ systematically from non-contributors.
Due to lack of available data, we were not able to include uninsured populations in this analysis.
This report presents an analysis of the prevalence of opioid use disorder in the United States as identified through diagnosis codes related to opioid abuse, dependence, or poisoning, without regard to prescription drug histories. There are likely additional patients with opioid use disorder who are not represented in this study who have prescription drug claims for opioid treatment therapies that do not have corresponding medical claims associated with an opioid use disorder diagnosis. The diagnosis codes used to identify opioid use disorder include a range of severities, including some cases of uncomplicated use and some in remission. Additionally, opioid poisoning doesn’t always happen within the context of an opioid use disorder.
Milliman has not audited any of the research data sets used for this analysis, but we have extensive experience working with them, and have found them to be reasonable. To the extent that there are errors or omissions in any of the data sources relied upon for this analysis, these results may also be in error. This report does not represent conclusive recommendations regarding treatment of opioid use disorder or legal advice. Milliman does not intend to benefit or create a legal duty to any recipient of this work.
Guidelines issued by the American Academy of Actuaries require actuaries to include their professional qualifications in all actuarial communications. Katie Matthews is a member of the American Academy of Actuaries, and meets the qualification standards for performing the analyses in this report.
Milliman did not receive any external funding for this analysis. Any opinions or views expressed in this report are those of the authors, not of Milliman.
The authors would like to thank Steve Melek and Anne Jackson for their helpful input and peer review of this material.
1Nahin, Richard L. (May 29, 2015). Estimates of Pain Prevalence and Severity in Adults: United States, 2012. Retrieved February 28, 2018, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4562413/.
2Siegel, M., Bradley, E.H., Kasl, S.V. (July-August 2003). Self-Rated Life Expectancy as a Predictor of Mortality: Evidence from the HRS and AHEAD Surveys. Retrieved February 28, 2018, from https://www.ncbi.nlm.nih.gov/pubmed/12792164.
3Kliff, S. (June 5, 2017). The opioid crisis changed how doctors think about pain. Retrieved February 28, 2018, from https://www.vox.com/2017/6/5/15111936/opioid-crisis-pain-west-virginia.
4Volkow, Nora D. (May 14, 2014). America’s Addiction to Opioids: Heroin and Prescription Drug Abuse. Retrieved February 28, 2018, from https://www.drugabuse.gov/about-nida/legislative-activities/testimony-to-congress/2016/americas-addiction-to-opioids-heroin-prescription-drug-abuse.
5CDC (2017). Annual Surveillance Report of Drug-related Risks and Outcomes. Retrieved February 28, 2018, from https://www.cdc.gov/drugoverdose/pdf/pubs/2017-cdc-drug-surveillance-report.pdf.
6Kaiser Family Foundation (2016). Opioid Overdose Death Rates and All Drug Overdose Death Rates per 100,000 Population (Age-Adjusted). Retrieved February 28, 2018, from https://www.kff.org/other/state-indicator/opioid-overdose-death-rates.
7CDC (December 19, 2017). Drug Overdose Death Data. Retrieved February 28, 2018, from https://www.cdc.gov/drugoverdose/data/statedeaths.html.
8Dowell, D. et al. (September 19, 2017). Contribution of opioid-involved poisoning to the change in life expectancy in the United States, 2000-2015. JAMA. Retrieved February 28, 2018, from https://jamanetwork.com/journals/jama/article-abstract/2654372.
9American Society of Addiction Medicine. Opioid Addiction 2016 Facts & Figures. Retrieved February 28, 2018, from https://www.asam.org/docs/default-source/advocacy/opioid-addiction-disease-facts-figures.pdf.
10Including ICD-9-CM codes beginning with 304.0, 304.7, 305.5, 965.0, and ICD-10-CM codes beginning with F11, T40.0, T40.1, T40.2, and T40.3.
11Thompson, D (August 1, 2017). More than 1 in 3 Americans prescribed opioids in 2015. CBS News. Retrieved February 28, 2018, from https://www.cbsnews.com/news/more-than-one-third-americans-prescribed-opioids-in-2015/.
12Population counts by age, state, and payer were developed from the 2016 Current Population Survey using the CPS Table Creator, available at https://www.census.gov/cps/data/cpstablecreator.html.
13Horowitz, E (May 2, 2016). US facing not one, but two opioid epidemics, Boston Globe. Retrieved February 28, 2018, from http://www.bostonglobe.com/metro/2016/05/01/facing-not-one-but-two-opioid-epidemics/66CMuMtPuKHtZPx7tOxsPM/story.html.
14Due to Medicaid data limitations, 2012 data were used for Kansas and Rhode Island, and the national average was used as an estimate for Colorado.
15Due to Medicaid data limitations, 2012 data were used for Kansas and Rhode Island, and the national average was used as an estimate for Colorado.
16Young K., Zur, J. (July 14, 2017). Medicaid and the Opioid Epidemic: Enrollment, Spending, and the Implications of Proposed Policy Changes. Kaiser Family Foundation. Retrieved February 28, 2018, from https://www.kff.org/medicaid/issue-brief/medicaid-and-the-opioid-epidemic-enrollment-spending-and-the-implications-of-proposed-policy-changes/.