Summary of individual market enrollment and Affordable Care Act subsidies
Executive summary
Following the introduction of the Patient Protection and Affordable Care Act (ACA), the individual health insurance marketplace has experienced continuous changes. To support understanding of the condition and stability of the individual market, we have prepared our third annual profile of the individual health insurance market for each state along with the District of Columbia (DC).
Profiles of the individual health insurance market for the 50 states and the District of Columbia
These state profiles summarize insurer financials, marketplace enrollment1, and federal assistance provided to households purchasing insurance coverage through the insurance marketplaces, incorporating recently released data from the 2019 open enrollment period 2 and estimated 2019 effectuated enrollment 3 . The table below summarizes our estimates of effectuated marketplace enrollment and associated federal financial assistance for calendar year (CY) 2016 through CY 2019 time period. Historical data has been updated based on published data subsequent to the release of previous reports.
As illustrated in the table, aggregate premium assistance expenditures materially increased between 2017 and 2018, but are estimated to slightly decrease from 2018 to 2019. These changes are primarily attributable to national composite subsidy benchmark premiums increasing by 34% in 2018, but declining by (1%) in 2019. 4 Assuming stable marketplace enrollment, federal premium assistance expenditures for 2020 are likely to continue to decline as a result of a (3%) subsidy benchmark premium decrease. 5 Premium rate decreases for 2019 and 2020 are partially attributable to several states implementing state-based reinsurance programs (as discussed below).
| 2016 | 2017 | 2018 | 2019 | |
| Average monthly marketplace enrollees | 10,007,000 | 9,763,000 | 9,895,000 | 9,842,000 |
| Average monthly premium subsidy recipients | 8,396,000 | 8,228,000 | 8,578,000 | 8,601,000 |
| Average monthly CSR subsidy recipients | 5,634,000 | 5,597,000 | 5,192,000 | 5,003,000 |
| Annual premium subsidy1 | $3,500 | $4,500 | $6,200 | $6,100 |
| Annual CSR subsidy payments1,2 | $1,000 | $1,000 | N/A | N/A |
| Aggregate premium subsidy ($ millions)3 | $29,228 | $36,836 | $53,279 | $52,887 |
| Aggregate CSR subsidy payments ($ millions)2 | $5,393 | $4,998 | N/A | N/A |
| Aggregate premium & CSR subsidy payments ($ millions) | $34,621 | $41,834 | $53,279 | $52,887 |
Notes
1.Values have been rounded and reflect estimated annual per capita amounts.
2. CSR subsidy payments reflect estimated benefits received by marketplace consumers prior to the discontinuation of CSR payments on October 12, 2017.6
a. Amounts exclude CSR subsidy payments provided to Medicaid-eligible consumers in Arkansas and New Hampshire, which were estimated to be approximately $500 million in 2016 and 2017.
b. Following the termination of CSR payments in 2017, premium rates have been increased by insurers to reflect the loss of direct federal CSR subsidy funding, resulting in an increase to premium subsidy amounts.
3. Aggregate premium subsidy amounts exclude federal pass-through funding related to 1332 Waiver approvals.
This information is vital to state, federal, and insurer stakeholders for several reasons:
-
1332 State Innovation Waiver (1332 Waiver).
The number of states with approved 1332 Waivers has increased from three in 2018 to 13 as of October 2019, with 12 of the approved 1332 Waivers including reinsurance provisions. 7 State-based reinsurance programs have become a common approach to adhering to 1332 Waiver requirements of covering at least as many individuals under current law, while not increasing the federal deficit. Under these programs, federal pass-through funding is generated from the reduction to federal premium subsidies provided to consumers. These programs also assist in enabling marketplace coverage to be more affordable for consumers not eligible for advanced premium tax credits (APTC).
In 2018, approximately $250 million in federal pass-through funding was provided to the three states operating a reinsurance program under a 1332 Waiver. 8 The amount of 1332 Waiver federal pass-through funding is expected to exceed $1 billion by 2020. Each state profile provides estimated federal expenditures on APTC and cost-sharing reduction (CSR) subsidies along with the number of individuals receiving these subsidies from CY 2016 through CY 2019. This information can enable a state to better understand the funding and coverage requirements that must be adhered to under Section 1332 of the ACA. - Insurer stability. On an aggregated basis, insurers reported financial losses in the individual market in CY 2010 9 through CY 2016, with CY 2017 marking the first year of financial gains in recent history. 10 Year-end financial reporting for CY 2018 suggests further financial improvement, with insurer margins approaching 10% of premium. Insurers’ return to profitability is anticipated to result in favorable premium changes in future years, with many states having experienced marketplace premium decreases in 2019 and minimal increases nationally for 2020. 11,12 The state profiles contain key financial metrics for CY 2017 and CY 2018, providing further insight into insurer financial stability in each market.
-
Marketplace enrollment.
Average monthly marketplace enrollment has remained stable in recent years, with minimal changes in the number of premium subsidy recipients between CY 2018 and CY 2019. However, during this same time period, the number of consumers receiving CSR subsidies has diminished. In many states, the population eligible for CSR subsidies have the ability to select a low cost (or often no cost) bronze-level plan as a result of CSR loading on silver-level plans 13 (resulting from the discontinuation of direct CSR funding effective October 201714 ). When selecting a bronze plan, the recipient forgoes CSR subsidies in lieu of lower upfront premium costs. Enrollment patterns in recent years have demonstrated that this is perceived as an attractive trade-off for many individuals.
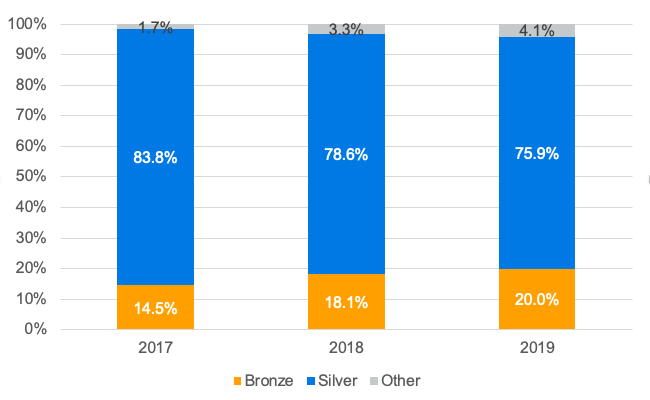
Bronze plans often have high member cost sharing requirements (capped at $7,900 and $15,800 for individual and family coverage, respectively, in 201915 ), which may exceed affordable levels for the low-income population electing to purchase bronze coverage over a CSR plan. This dynamic has the potential to result in increases in provider bad debt and other related expenses. Each state profile includes information related to the number of individuals receiving premium subsidies and CSR subsidies over time, which can assist stakeholders in understanding the extent to which this could be occurring in a given market. The figure below illustrates changes in the distribution of marketplace selections by metal level for persons with income between 100% and 250% of the federal poverty level (FPL). Bronze-level selections have increased from approximately 15% of total plan selections in 2017 to 20% in 2019.
Figure 1: Metal Level Selections for Persons with income between 100% and 250% FPL
Note: Data reflects only states reporting metal-level household income data for the Centers for Medicare and Medicaid Services (CMS) marketplace open enrollment report in each year. - Marketplace premium. Marketplace premium changes from 2016 to 2019 varied by state due to a number of factors, including insurer profitability, risk pool morbidity, the treatment of CSR payment termination 16 , and the availability of reinsurance through one of the approved 1332 Waivers. States with high insurer profits in CY 2018 or recently approved 1332 Waivers are likely to have experienced low, or even negative, marketplace premium increases in CY 2019. Figure 1 and Figure 3 of our state profiles provides insight into this dynamic.
Methodology and assumptions
The information contained in this report and the 51 state market profiles was prepared through the use of publicly available data sources and estimates of effectuated marketplace enrollment. Effectuated marketplace enrollment includes the population that has made premium payments and is actively enrolled in a marketplace policy. Data underlying our analyses is based on information from CY 2016 through CY 2019.
Insurer financial results
Financial results for CY 2017 were summarized through the use of annual Medical Loss Ratio Reporting Data (MLR Data), which was publicly released by the Center for Consumer Information and Insurance Oversight (CCIIO) within CMS. 17 Financial results for 2018 were based on statutory statement financial data submitted through the National Association of Insurance Commissioners’ Supplemental Health Care Exhibit (SHCE). SHCE data was not available for California and Massachusetts because a material number of companies operating in these markets do not complete NAIC statutory financial statements. Individual market financial information from the MLR and SHCE Data is inclusive of marketplace enrollment, off exchange (marketplace) enrollment, and enrollment on transitional products. Further information related to CY 2017 and CY 2018 insurer financial results can be found in our annual research report on the commercial health insurance market. 18 Additional adjustments were made to the data for observed reporting issues or data variances relative to statutory financial statements.
Marketplace enrollment and subsidy value
CMS released effectuated enrollment summaries for the insurance marketplace on a national and state level for 2016 through 2019. 19,20,21 Effectuated marketplace enrollment was provided separately for total marketplace enrollment, APTC enrollment, and CSR enrollment.
- APTC:Payments are made directly to the insurance company by the federal government on behalf of the qualifying members to make out-of-pocket premiums more affordable for lower-income households. The amount of the premium tax credit varies for each qualifying household based on its income relative to the FPL and the price of the second-lowest-cost silver plan (commonly known as the “subsidy benchmark plan”) that the household can purchase in the insurance marketplace. Qualifying households must have income between 100% and 400% of the FPL and must not be eligible for other sources of affordable minimum value coverage.
- CSR:The ACA requires insurers participating in the individual insurance marketplace to automatically provide a reduced level of cost sharing to qualifying households. Reduced cost sharing takes the form of CSR variations of base silver plans on the marketplace. The CSR variants include reductions to cost sharing such as deductibles, copayments, coinsurance, and out-of-pocket maximums. The magnitude of the reduction to required plan cost sharing varies based on the income level of the qualifying households purchasing such coverage. Qualifying households must have income between 100% and 250% 22 of the FPL and must not be eligible for other sources of affordable minimum value coverage.
The effectuated marketplace enrollment data also includes the average APTC on a national and state level. We relied on CY 2019 marketplace open enrollment report (OER) public use file to estimate the average premiums for members receiving a premium subsidy.
For CY 2016 through 2019, average monthly premium (for individuals receiving an APTC) were estimated through the use of the public use files for states using the federal marketplace. Due to inconsistent data sources across the three-year period, we have not illustrated monthly marketplace premiums for state-based exchanges that operated in 2019. For all states, it is certain that the actual results will vary from the estimates developed within each state profile. CSR payments were sourced from the MLR Data. For Arkansas and New Hampshire, we adjusted the CSR payments reported in the MLR data for private Medicaid expansion enrollees.
Data reliance
Publicly available data used in our analysis was reviewed for reasonableness and consistency. However, the data sources have not been audited. To the extent data items were not correctly reported, the values presented in this report and accompanying state profiles will need to be updated.
1Marketplace enrollment is limited to the federally facilitated and state insurance marketplaces.
2“2019 Marketplace Open Enrollment Period Public Use Files.” Retrieved on June 21, 2019, from https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/Marketplace-Products/2019_Open_Enrollment.html
3“Early 2019 Effectuated Enrollment Snapshot.” Retrieved on August 13, 2019, from https://www.cms.gov/sites/default/files/2019-08/08-12-2019%20TABLE%20Early-2019-2018-Average-Effectuated-Enrollment.pdf
4“Marketplace Average Benchmark Premiums.” Retrieved on November 1, 2019, from https://www.kff.org/health-reform/state-indicator/marketplace-average-benchmark-premiums/.
6“Payments to Issuers for Cost-Sharing Reductions (CSRs).” Retrieved on October 10, 2019, from https://www.hhs.gov/sites/default/files/csr-payment-memo.pdf
7“Tracking Section 1332 State Innovation Waivers.” Retrieved on October 10, 2019, from https://www.kff.org/health-reform/fact-sheet/tracking-section-1332-state-innovation-waivers/
8The following states operated a reinsurance program under a 1332 Waiver in 2018: Alaska, Oregon, and Minnesota.
9CY 2010 was the first year that health insurers completed the National Association of Insurance Commissioners (NAIC) Supplemental Health Care Exhibit, providing greater detail and visibility into state-level commercial market financial results.
10 “Commercial health insurance: Detailed 2017 financial results and emerging 2018 trends.” Retrieved on October 10, 2019, from https://www.milliman.com/insight/2019/Commercial-health-insurance-Detailed-2017-financial-results-and-emerging-2018-trends/
11“2019 Premium Changes on ACA Exchanges.” Retrieved on May 1, 2019, from https://www.kff.org/health-costs/issue-brief/tracking-2019-premium-changes-on-aca-exchanges/
12 “Premiums for HealthCare.gov Plans are down 4 percent but remain unaffordable to non-subsidized consumers.” Retrieved on October 22, 2019, from https://www.cms.gov/newsroom/press-releases/premiums-healthcaregov-plans-are-down-4-percent-remain-unaffordable-non-subsidized-consumers
13See https://www.modernhealthcare.com/article/20180405/NEWS/180409943/is-silver-loading-the-silver-bullet-actuaries-wary-of-long-term-impact-of-csr-cutoff for more information.
14 “Trump Administration Takes Action to Abide by the Law and Constitution, Discontinue CSR Payments.” Retrieved on November 1, 2019, from https://www.hhs.gov/about/news/2017/10/12/trump-administration-takes-action-abide-law-constitution-discontinue-csr-payments.html
15 “Patient Protection and Affordable Care Act; HHS Notice of Benefit and Payment Parameters for 2019.” Retrieved on October 10, 2019, from https://www.federalregister.gov/documents/2018/04/17/2018-07355/patient-protection-and-affordable-care-act-hhs-notice-of-benefit-and-payment-parameters-for-2019
16 Additional information related to the treatment of CSR payment termination can be found at https://www.balloon-juice.com/2017/10/11/state-approaches-to-handling-csr-uncertainty-for-2018-premiums/
17 CMS. Medical Loss Ratio Data and System Resources. CCIIO. Retrieved on May 1, 2019, from https://www.cms.gov/CCIIO/Resources/Data-Resources/mlr.html
18 “Commercial health insurance: Detailed 2017 financial results and emerging 2018 trends.” Retrieved on November 25, 2019, from https://www.milliman.com/insight/2019/Commercial-health-insurance-Detailed-2017-financial-results-and-emerging-2018-trends/
19 “2017 Effectuated Enrollment Snapshot” by CMS. June 12, 2017. Retrieved on June 21, 2019, from https://downloads.cms.gov/files/effectuated-enrollment-snapshot-report-06-12-17.pdf
20 “Early 2018 Effectuated Enrollment Snapshot” by CMS. July 2, 2018. Retrieved on June 21, 2019, from https://www.cms.gov/CCIIO/Programs-and-Initiatives/Health-Insurance-Marketplaces/Downloads/2018-07-02-Trends-Report-1.pdf
21 “Early 2019 Effectuated Enrollment Snapshot.” Retrieved on August 13, 2019, from https://www.cms.gov/sites/default/files/2019-08/08-12-2019%20TABLE%20Early-2019-2018-Average-Effectuated-Enrollment.pdf
22 Native Americans with income up to 300% FPL are also eligible for 100% CSR plans.
23 “2019 Marketplace Open Enrollment Period Public Use Files.” Retrieved on June 21, 2019, from https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/Marketplace-Products/2019_Open_Enrollment.html
Explore more tags from this article
About the Author(s)
Summary of individual market enrollment and Affordable Care Act subsidies
These state profiles summarize insurer financials, marketplace enrollment, and federal assistance provided to households purchasing insurance coverage through the insurance marketplaces, incorporating recently released data from the 2019 open enrollment period and estimated 2019 effectuated enrollment.